Researchers progress toward AIDS vaccine

Rutgers AIDS researchers Gail Ferstandig Arnold and Eddy Arnold may have turned a corner in their search for a HIV vaccine. In a paper just published in the Journal of Virology, the husband and wife duo and their colleagues report on their research progress.
With the support of the National Institutes of Health, the Arnolds and their team have been able to take a piece of HIV that is involved with helping the virus enter cells, put it on the surface of a common cold virus, and then immunize animals with it. They found that the animals made antibodies that can stop an unusually diverse set of HIV isolates or varieties.
Some researchers have previously been able to elicit effective antibodies, but usually only against a very limited number of HIV types. With HIV’s known propensity to mutate, antibodies developed against one local strain may not recognize and combat mutant varieties elsewhere. These geographic varieties with different mutations constitute one of the great challenges to finding a broad spectrum vaccine capable of protecting against the vast array of HIV varieties.
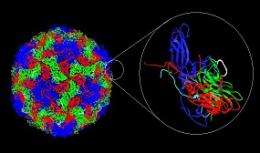
The approach taken by the Arnolds and their colleagues has been to identify a part of the AIDS virus that is crucial to its viability - something the virus needs in order to complete its life cycle - and then target this Achilles heel.
“The part that we targeted plays a role in the ability of HIV to enter cells, and is common to most HIV varieties,” Gail Ferstandig Arnold said. “That is a mechanism that would not be easy for the virus to reinvent on the fly, so it turns out to be a really helpful target.”
The Arnolds are both members of the Center for Advanced Biotechnology and Medicine, a joint center of Rutgers, The State University of New Jersey, and the University of Medicine and Dentistry of New Jersey. Also, Gail Ferstandig Arnold is a research professor and Eddy Arnold is a professor, both in Rutgers’ Department of Chemistry and Chemical Biology.
While most vaccines are actually made from the pathogen itself, employing weakened or inactivated organisms to stimulate antibody production, HIV is just too dangerous to use as the basis for a vaccine vehicle. What the Arnolds have done is to use the relatively innocuous cold-causing rhinovirus and attach the target portion of the HIV. This must be done in a way that maintains the HIV part’s shape so that when the immune system sees it, it will actually mount an immune response as it would to the real HIV.
“The idea is to trick the immune system into thinking it is acting upon HIV before the virus shows actually shows up on the scene,” said Eddy Arnold.
To actually accomplish this is a big problem in engineering. The goal was to take a small piece of the HIV out of its native context, put it in a completely different system (rhinovirus), and have it look the same and act the same. Eddy Arnold likens this to taking the Rocky Mountains, putting them on India and having them look exactly right.
Using recombinant engineering, the research team developed a method to systematically test millions of varied presentations of the HIV segment with the rhinovirus. They tried millions of different variations on how to graft (or splice) one onto the other, creating what are called combinatorial libraries.
“It’s like the lottery,” Eddy Arnold commented. “The more tickets you buy the better chance you have of winning.”
“The really exciting part is that we were able to find viruses that could elicit antibodies against a huge variety of isolates of HIV. That is an immense step and a very important step,” said Gail Ferstandig Arnold.
“However, we need to be careful to not overstate things because the quantity of response is not huge, but it is significant,” added Eddy Arnold. “This is actually the first demonstration of this particular Achilles heel being presented in way to generate a relevant immune response. It is probably not potent enough by itself to be the vaccine or a vaccine, but it is a proof of principle that what we are trying to do is a very sound idea.”
Source: Rutgers University (news : web)















