Scientists report breakthrough in HPV research
University of Alabama at Birmingham researchers have developed a new, inexpensive and efficient method for producing and studying a type of human papillomavirus (HPV) that causes cervical cancer. The process could speed understanding of how the virus functions and causes diseases, and lead to new prevention or treatment options.
In findings reported on-line and in print in January in Genes & Development, the UAB team detailed a process for producing HPV-18 in the laboratory. Previously, the virus had proven resistant to propagation in a lab setting, making it extremely difficult for scientists to study the virus and its effects on the host cells that it infects.
"The old method for propagating papillomaviruses in the lab for study was compromised by several factors," said Louise Chow, Ph.D., professor of biochemistry and molecular genetics at UAB and a study co-author. "We could only look at the viral DNA gene by individual gene, which gave us little insight into how the entire virus coordinated its replication program or how it interacted with the host cells and tissues that had been infected."
The new method, which Chow and study co-author Thomas Broker, Ph.D., professor of biochemistry and molecular genetics, have been developing for over 20 years, for the first time allows researchers to reproduce the entire infection cycle of HPV-18 in primary human skin cells, called keratinocytes. The breakthrough is the result of several years of intensive and creative efforts by graduate students Hsu-Kun (Wayne) Wang and Aaron Duffy, coauthors of the publication. Scientists now can observe how the virus behaves in the same cells it would infect in a human body.
"This system provides marvelous opportunities to understand how HPV works on a very basic, molecular level," Broker said. "The ongoing research will reveal promising targets for drug design, better understanding of how the new prophylactic HPV vaccines block infection and, for the first time, offer real hope that we can find a way to combat a virus that potentially affects 80 to 85 percent of women in the world, through therapeutic treatment of established infections."
Chow and Broker say the old method for producing HPV cells suffered from several factors, including the need to use bacterially derived recombinant DNA to introduce the viral DNA into skin cells. The presence of bacterial DNA sequences altered the HPV DNA so that it no longer closely resembled the natural viral structures found in human infections. Their new method generates circular viral genomes in the cells with high efficiency, and these can go on to replicate autonomously, without complications associated with the usual gene transfer vectors.
Another stumbling block was the need to use immortalized host cells to grow HPV. Immortalized cells have been genetically altered to live indefinitely and they do not differentiate properly into full-thickness skin tissue. While the use of immortalized cells as a host allowed the viral genome to be studied gene by gene, immortalized cells do not resemble the actual primary cells found in the body, preventing meaningful observations of how HPV functions in normal human host cells.
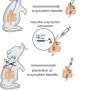
The new method also uses technology developed for skin grafting. It involves isolating primary human keratinocytes from foreskin removed during circumcision. The cells are grown in a 'raft' culture held at the liquid medium-air interface until they stratify, differentiate, and reach the thickness of normal epithelia, forming sheets of tissue virtually indistinguishable from real skin. If the viral DNA is introduced into the keratinocytes before they are placed into the raft culture environment, it carries out its full reproductive program including controlled RNA transcription, DNA replication, and packaging into the capsid proteins, as it would in the human body. Such progeny viruses are then capable of reinfecting fresh skin cells and repeating the entire infection cycle.
Currently there is no non-surgical treatment for HPV-associated lesions, and the current research in the Chow-Broker laboratory is focused on identifying inhibitors of essential viral activities so that antiviral agents can be developed to treat existing infections, either post-operatively or without any need for surgery.
HPV-18 is the only strain of the papillomavirus that the Chow-Broker lab has reproduced using the new method, but they say it should work on other HPV types. There are at least 120 different strains of HPV. While most are relatively harmless skin viruses, there are some, like HPV-18, that are linked to genital warts, dysplasias, and cervical and penile cancers and certain oral cancers. Such lesions can be identified using Pap smear cytology or new more sensitive and accurate molecular tests.
"HPV is part of the human condition," Broker said. "Virtually every adult in the world has been infected with HPV at some point in their life. Many of us will have no ill effects. Nonetheless nearly 1,000 women die each day from cervical cancer worldwide. Many victims are relatively young, and this preventable disease takes away about 30 years of life expectancy and leaves families without their wife and mother."
A vaccine is available that provides protection from the four HPV strains most associated with cervical cancer and genital warts. The vaccine is recommended for girls age 9-12 and can be given to women up to 26 years of age. Studies are ongoing to determine whether the vaccine prevents HPV infection in males.
"While we are very fortunate to have the HPV vaccine, there are holes in our understanding of how it works," Chow said. "Using our new method, we will be able to see how vaccine-induced antibodies actually prevent infection, and this could lead to a better understanding of how the vaccine works…and potentially to better vaccines."
Source: University of Alabama at Birmingham