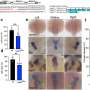
'Normalizing' tumor vessels leaves cancer more benign
A report publishing online on February 12th in the journal Cell, a Cell Press publication, suggests a counterintuitive new method to make cancer less likely to spread: by normalizing the shape of tumors' blood vessels to improve their oxygen supply. Such a treatment strategy might also boost the efficacy and reduce resistance to available anti-cancer drugs and so-called anti-angiogenic drugs that work by cutting off the growth of new blood vessels.
"In tumors, the endothelial cells lining blood vessels grow in all directions and over each other," said Peter Carmeliet of Vesalius Research Center. Irregular shape and gaps left in the vessel walls also make them leaky.
Tissues need oxygen delivered by the bloodstream to grow. But, in the case of tumors, that haphazard overgrowth of blood vessels and deteriorated endothelial lining impairs their own ability to function, he continued. As a result, tumors become more and more oxygen deprived - a condition that is a "driving force" for cancer cells to escape and spread to other parts of the body.
That vicious cycle might be halted with treatments designed to target an oxygen-sensing enzyme known as PHD2 in the linings of tumors' blood vessels, Carmeliet's team now finds. The new results also offer fundamental new insight into blood vessel biology.
Indeed, numerous earlier studies had examined how blood vessels arise, branch and elongate at the molecular level. However, little was known about how vessels regulate their shape.
Since supply of oxygen is one of the most basic functions of vessels, the researchers also suspected that they should possess ways to sense and re-adapt oxygen supply in the case of a shortage. They looked to a newly discovered class of oxygen sensors: the prolyl hydroxylase domain proteins, PHD1-3.
In the current study, Carmeliet's group focused on the role of PHD2 in balancing oxygen levels by influencing the characteristics of blood vessels. In mice with half the normal amount of PHD2 in the endothelial cells that line blood vessels, tumor vessels were found in the same numbers and sizes. However, the shape and structure of those vessels was more "normal," with linings made up of tightly aligned, orderly shaped and smooth cells having a cobblestone appearance.
That more regular vessel structure improved tumors' oxygen supply, leading to physiological changes that counteracted the overall malignancy of the cancer, they report. The cells were better able to counterbalance the "abnormalizing" effects of the tumors, and halt the progression to metastasis.
The findings in mice may have medical implications. "By normalizing the tumor vasculature, partial loss of PHD2 may shift tumors from an aggressive metastasizing tumor type to a more benign, well-encapsulated tumor," the researchers said. The partial loss of PHD2 doesn't seem to affect the blood vessels of healthy tissues, they said, suggesting a PHD2 inhibitor might selectively target tumor vessels.
Working to keep a tumor well-supplied with a key nutrient like oxygen may seem counterintuitive, but such a therapy might also be an advantageous addition to existing treatment regimens, Carmeliet added, noting that chemotherapeutic drugs and radiation depend on adequate oxygen levels to work. Targeting PHD2 might also help to avoid a potential pitfall of anti-angiogenic drugs that attempt to "starve" tumors by pruning back their blood vessel supply. "You have to be careful," he said. "If you prune too many vessels, leaving tumors overly hypoxic, it may induce their resistance."
Source: Cell Press