Call to action: Running out of options to fight ever-changing 'super bugs'
People are dying from "super bugs" because our antibiotic arsenal has run dry, leaving the world without sufficient weapons to fight ever-changing bacteria, warn infectious disease researchers at The University of Texas Medical School at Houston.
In a Jan. 29 perspective in The New England Journal of Medicine, Barbara E. Murray, M.D., and Cesar Arias, M.D., Ph.D., evaluate the past, present and future response to preventing and treating "super bugs."
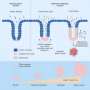
A "super bug" is an organism that is resistant to antibiotics. It can evade antibiotics by:
• destroying the medication by producing an enzyme that devours the drug;
• creating a barrier to the drug;
• pumping out any antibiotic that reaches the bacterial cell;
• modifying the target of the antibiotic so the drug can't bind to it.
"Most of the public has heard of MRSA (methicillin-resistant Staphylococcus aureus) because it produces the most cases each year. However, they have not heard of other super bugs that can be far worse," said Murray, co-author and director of Division of Infectious Diseases at the UT Medical School. "The Gram-negative bacteria are the most antibiotic-resistant with fewer treatment options in life-threatening diseases, such as certain forms of pneumonia, bloodstream infections, gastroenteritis and even meningitis." Gram-negative bacteria can release toxins created by their cell walls into the bloodstream, where it is harder to treat them.
According to a 2004 report, "Bad Bugs, No Drugs," by the Infectious Diseases Society of America (IDSA), none of the 89 new drugs approved by the U.S. Food and Drug Administration were antibiotics. Murray and Arias say people are also taking antibiotics without prescriptions or not following the prescription as directed. It is those practices that allow the antibiotics to be exposed to a wide-range of bacteria in the body, both good and bad, which gives the bugs an opportunity to find ways to beat antibiotic weapons.
"We have run out of options. The promise of genomics has not panned out. Gene sequencing has not helped us find a better way to fight these bugs," said Murray, holder of the J. Ralph Meadows Professorship in Internal Medicine at the medical school. Genomics is the study of an organism's genomes to chart its DNA sequencing.
According to the IDSA's 2004 report, the research on new antibiotics is simply drying up, in part due to the expense of bringing a new drug to market. "The pharmaceutical companies, like all other publicly traded industries, must deliver to its shareholders in order to justify their continued investment. The unique nature of antibiotics makes securing investments challenging. Because antibiotics work so well and so fast, they produce a weak return on investment for manufacturers. Antibiotics are commonly prescribed for seven to 14 days," the report said.
"Academics can't do it all. Pharmaceutical companies can't do it all. Everyone needs to work together to address this potential worldwide public health crisis," said Arias, co-author of the perspective and assistant professor in infectious diseases at the medical school.
Delay in diagnosis is also an issue. Murray said even with advancements, it takes about 48 hours or more from the time a culture is taken to determine what a person may have contracted and to determine what antibiotics are likely to be effective. "It may not sound like a lot of time, but with some of these bugs you have to move quickly to save a patient. You don't want the bacteria to spread. Research needs to include finding new testing methods," Murray said.
The Division of Infectious Diseases at the UT Medical School is already working toward solutions. It has now established the Laboratory for Antimicrobial Research, headed by Arias, within the Center for the Study of Emerging and Re-Emerging Pathogens, headed by Murray. The laboratory, which is supported with funding from the National Institutes of Health (NIH), aims to investigate the clinical and molecular aspects of antibiotic resistance, attempting to understand the complex mechanisms by which bugs become resistant to antibiotics and then designing new strategies to combat them.
Source: University of Texas Health Science Center at Houston