Clue to genetic cause of fatal birth defect
A novel enzyme may play a major role in anencephaly, offering hope for a genetic test or even therapy for the rare fatal birth defect in which the brain fails to develop, according to a study from researchers at the University of Illinois at Chicago College of Medicine.
The study appears in the October issue of the journal of Molecular Endocrinology.
In the U.S., 1,000 to 2,000 children are born with anencephaly each year. Most do not survive more than a day or two. Although anencephaly can sometimes be diagnosed through ultrasound, which picks up the malformation of the head, there is no genetic test, and its cause is unknown.
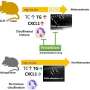
By breeding special "knockout" mice that were missing the gene for the enzyme called HSD17b7, UIC researchers found that such mice died on the tenth day of gestation with the severe lack of brain development that characterizes the human birth defect.
The failure of the mice to develop, as well as the extreme nature of the changes in the formation of the animals, was very surprising, said Geula Gibori, UIC distinguished professor of physiology and biophysics and principal investigator of the study. Mice that lack enzymes of similar function are born with subtle changes in their cognitive ability, but they survive.
The UIC researchers had previously discovered this novel enzyme and were focused on its role in converting the weak hormone estrogen into the more potent estradiol in the ovaries and its possible role in breast cancer.
Recent research has shown that the HSD17b7 enzyme has an additional role in the last steps of cholesterol biosynthesis. But because the fetus receives cholesterol from the mother during gestation, Gibori and her colleagues did not expect the enzyme to be of much importance to development, she said.
However, it appears that as the fetal mouse brain develops it forms a blood barrier, blocking maternal cholesterol from brain cells. The brain becomes dependent on the biosynthesis of its own cholesterol once this blood-brain barrier forms, at day 10 of gestation.
The UIC researchers established that in the fetus, the brain is the most important site for HSD17b7 expression and provided evidence that anencephaly may result from the loss of this enzyme.
"Creating a knockout mouse is a very laborious process," said Aurora Shehu, first author of the paper and at that time a graduate student in Gibori's laboratory. Mice with only one copy of the gene are produced and then interbred; one in four of their offspring should have no copy of the gene -- a "null" mouse.
"We expected null mice to be born and to be infertile, however, no null mice were born," said Shehu. "I was afraid I had made a mistake, and went back to the beginning, repeating the entire process, but still no null mice were born."
Shehu then began more painstaking work, performing in-utero genetic testing on entire litters -- often 10 to 12 fetuses per litter. She found that the null mice were there, but they were dying at day 10 of gestation, when the blood-brain barrier develops.
Gibori says the gene that is missing or defective in human anencephaly is not yet known, but the discovery that the deletion of HSD17b7 in the mouse causes anencephaly suggests this gene may be awry in the human disease.
"This opens up very exciting possibilities for understanding human anencephaly, and, perhaps, someday being able to provide a genetic test for the condition early in pregnancy -- and ultimately a therapy," she said.
As their next step, Gibori's lab plans to test human anencephalic tissue for a mutation in the HSD17b7 gene.
Source: University of Illinois at Chicago