Rodent studies suggest mother's diet can affect genes and offspring's risk of allergic asthma
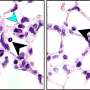
A pregnant mouse's diet can induce epigenetic changes that increase the risk her offspring will develop allergic asthma, according to researchers at National Jewish Health and Duke University Medical Center. Pregnant mice that consumed diets high in supplements containing methyl-donors, such as folic acid, had offspring with more severe allergic airway disease than offspring from mice that consumed diets low in methyl-containing foods. The results of the study are being published Sept. 18, 2008, in the online version of the Journal of Clinical Investigation and will appear in the October print issue.
"Our findings suggest that a mother's diet that alters DNA methylation can affect the development of the fetus's immune system, predisposing it to allergic airway disease," said David Schwartz, MD, senior author on the paper and Professor of Medicine at National Jewish Health. "It also suggests the dramatic increase in asthma during the past two decades may be related in part to recent changes in dietary supplementation among women of childbearing age."
The prevalence of asthma has nearly doubled in the past 25 years. Asthma currently affects about 11 percent of the US population and accounts for $9.4 billion in direct healthcare costs. Although both genes and environment are believed to play a role in the development of asthma, scientists have been unable to definitively identify specific causes of the disease or explain the rise in prevalence.
Epigenetics is the study of gene regulation. Environmental exposures can lead to modification of methyl groups (CH3) binding to certain DNA molecules, which can result in modified expression of specific genes. A variety of environmental factors, including diet, tobacco smoke, and medications, can modify methyl groups binding to DNA, particularly during periods of vulnerability. Although no changes occur in the genetic code, epigenetic effects can be passed to offspring. Emerging research has indicated that epigenetic mechanisms can affect the development of the immune system, skewing it either toward or away from a predisposition to allergies.
The research team decided to examine the potential role of epigenetics in the development of allergic asthma. They fed pregnant mice diets either high or low in methyl donors. In addition to folic acid, the high methyl-donor diets additionally contained higher levels of L-methionine, choline, and genistein.
When the researchers evaluated offspring mice using a model of allergic asthma, they found that mice, whose mothers had the high methyl-donor diets, showed greater severity of asthma; more airway hyperreactivity, more allergic inflammation in their airways, and higher levels of the IgE in their blood. They also found that T cells were more likely to be the type associated with allergy.
The male offspring also transmitted a higher predisposition to allergic airway disease to their progeny. In contrast, mice exposed to high-methyl-donor diets during lactation or adulthood showed no increased propensity to allergic sensitization.
"There seems to be a crucial stage, during development in utero, when a young mouse is susceptible to epigenetic changes that can alter its immune system," said co-author John W. Hollingsworth, Assistant Professor of Medicine at Duke University School of Medicine. "These epigenetic changes may partially explain why it has been so difficult to definitively identify genes that contribute to asthma risk; the effect of genetic variations can be masked or further complicated by epigenetic changes."
When the researchers analyzed the genomes of the mice, they identified 82 genes that were significantly more methylated in high-methyl-diet (HMD) mice. The 10 most methylated genes were biologically plausible causes of asthma. These genes were transcription factors, which control the expression of many genes, and genes associated with cellular migration and allergic airway disease. The highly methylated genes were expressed at lower levels than less-methylated genes in mice receiving the low-methyl-donor diets.
The current research suggests too much folic acid (and other dietary supplements) during pregnancy may be related to an increased risk of allergies and asthma, and may even play a role in the dramatic increase in asthma prevalence during the past two decades. The U.S. Public Health service recommended in 1992 that all women of childbearing age consume 400 micrograms of folic acid daily to reduce their risk of birth defects of the spine and brain. In 1996 the U.S. Food and Drug Administration required that folic acid be added to specific flour, breads and other grains to prevent birth defects. Research has suggested that these measures have helped reduce birth defects.
Given the important role folic acid supplementation has played in prevention of birth defects, Drs. Schwartz and Hollingsworth do not advise any changes in folic acid supplementation, but do believe the issue is worth further investigation.
Source: National Jewish Medical and Research Center