Why some primates, but not humans, can live with immunodeficiency viruses and not progress to AIDS
Key differences in immune system signaling and the production of specific immune regulatory molecules may explain why some primates are able to live with an immunodeficiency virus infection without progressing to AIDS-like illness, unlike other primate species, including rhesus macaques and humans, that succumb to disease.
Following the identification of HIV (Human Immunodeficiency Virus) as the cause of AIDS 25 years ago, an extensive search was undertaken to identify the source of the virus. These studies led to the discovery that chimpanzees and sooty mangabeys are infected in the wild with simian immunodeficiency viruses (SIV), whose transmission to humans and macaques leads to AIDS.
Surprisingly, the natural hosts for the AIDS viruses, such as the mangabeys and numerous other African primate species who have been found to harbor SIVs in the wild, remain healthy despite infection. Understanding how the natural hosts evolved to resist the development of immunodeficiency disease has long represented a key unsolved mystery in our understanding of AIDS. Furthermore, definition of the mechanisms by which they resist disease could help explain the mechanisms underlying AIDS progression in humans.
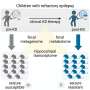
A team of scientists from Yerkes National Primate Research Center and the Emory Vaccine Center has discovered that the immune systems of sooty mangabeys are activated to a significantly lower extent during SIV infection than are the immune systems of rhesus macaques, and that this difference may explain why SIV and HIV infection leads to AIDS in some primate species but not others.
"During both HIV infection in humans and SIV infection in macaques, the host immune system becomes highly activated, experiences increased destruction and decreased production of key immune effector cells and progressively fails as a result. In contrast, natural hosts for SIV infection, like sooty mangabeys, do not exhibit aberrant immune activation and do not develop AIDS despite high levels of ongoing SIV replication. Our studies sought to understand the basis for the very different responses to AIDS virus infections in different species," says Mark Feinberg, MD, PhD, the paper's senior author. Feinberg is a former investigator at the Emory Vaccine Center and the Yerkes Research Center and a professor of medicine at the Emory University School of Medicine. He currently serves as vice president of medical affairs and policy for vaccines and infectious diseases at Merck & Co., Inc.
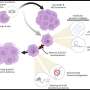
The reasons are found in significant differences in immune signaling in a specific type of dendritic cells in AIDS-susceptible or resistant host species. Dendritic cells are part of the immune system that play a key role in alerting the body to the presence of invading viruses or bacteria, and in initiating immune responses that enable clearance of these infections. They detect the invaders using molecules called Toll-like receptors.
Feinberg's team found that in sooty mangabeys, dendritic cells produce much less interferon alpha--an alarm signal to the rest of the immune system--in response to SIV. As a result, the dendritic cells are not activated during the initial or chronic stages of SIV infection, and mangabeys fail to mount a significant immune response to the virus. In contrast to mangabeys, dendritic cells from humans and macaques that are susceptible to developing AIDS are readily activated by HIV and SIV.
The difference in whether or not dendritic cells become activated upon AIDS virus exposure in specific primate hosts appears to result from species-specific differences in patterns of Toll-like-receptor signaling. Because host immune responses are unable to clear AIDS virus infections, ongoing virus replication leads to unrelenting activation of the immune system in humans and macaques.
Unfortunately, rather than promoting clearance of the infection, chronic dendritic cell stimulation may result in chronic immune activation and significant unintended damage to the immune system in AIDS-susceptible species. Such chronic immune activation is now recognized to be a major driving force for the development of AIDS.
The observation that mangabey dendritic cells are less susceptible to activation by SIV may explain why mangabeys do not exhibit abnormal immune activation and do not develop AIDS. Thus, in mangabeys, the generation of a less vigorous immune response to SIV may represent an effective evolutionary response to a virus that is so resistant to clearance by antiviral immune responses.
The authors suggest new treatment strategies that would steer the immune system away from over-activation, thereby protecting against the unintended damage caused by host immune responses. Such treatment approaches that focus on the host response to the AIDS virus may provide a valuable means of complementing the use of antiretroviral drugs that focus directly on inhibition of virus replication.
Understanding the particular details of Toll-like receptor signaling pathways in the mangabeys may help guide the development of specific therapeutic approaches that could beneficially limit chronic immune activation in HIV-infected humans.
"Better understanding of the biological basis by which sooty mangabeys and the numerous primate species that represent natural hosts for AIDS virus infections have evolved to resist disease promises to teach us a great deal about the emergence of the AIDS pandemic, and about the mechanisms underlying AIDS progression in humans. In addition, such insights will hopefully help inform new approaches to treat HIV infection most effectively." Feinberg says.
"Also, better understanding how natural hosts for SIV remain healthy may provide clues as to the future evolutionary trajectory of human populations in response to the profound selective pressures now being felt in regions of the world where the tragic consequences of HIV infection are most severe."
Reference: Nature Medicine advance online publication: Divergent TLR7 and TLR9 signaling and type I interferon production distinguish pathogenic and nonpathogenic AIDS virus infections.
Source: Emory University