Embryonic stem cells might help reduce transplantation rejection
Researchers have shown that immune-defense cells influenced by embryonic stem cell-derived cells can help prevent the rejection of hearts transplanted into mice, all without the use of immunosuppressive drugs.
The University of Iowa and the Iowa City Veterans Affairs (VA) Medical Center finding has implications for possible improvements in organ and bone marrow transplantation for humans. The study results appeared Friday in the online journal PLoS ONE, published by the Public Library of Science, at http://dx.plos.org/10.1371/journal.pone.0003212.
People who need bone marrow or solid organ transplantation must take immunosuppressive drugs that can cause side effects nearly as severe as the disease they have. They also can experience graft-versus-host disease, which can cause death.
These problems are spurring researchers to develop methods to reduce transplantation rejection, said the study's principal investigator Nicholas Zavazava, M.D., Ph.D., professor of internal medicine and director of transplant research at the UI Roy J. and Lucille A. Carver College of Medicine.
"The idea behind the study is to 'prep' a recipient's immune system to make it receptive to the eventual organ or bone marrow donor's genetic make-up," said Zavazava, who also is a researcher and staff physician with the Iowa City VA Medical Center. "The approach involves taking embryonic stem cells with the same genetic background as the donor from which the organ or bone marrow ultimately will come and adapting them into another type of stem cell that can be injected into the recipient."
Specifically, the team treated mouse embryonic stem cells with a "cocktail" of growth factors, causing them to become blood stem cells. These cells express very low levels of so-called "transplantation antigens" and are therefore protected from immunological rejection.
The researchers then injected the blood stem cells into the recipient mouse's blood circulation. These stem cells found their way into the recipient mouse's thymus, where, as happens in humans, the recipient's own bone marrow cells typically migrate and develop into immune-defense cells known as T-cells.
With the donor-related blood stem cells now present in the thymus, the mouse recipient's own T-cells learned to recognize them as part of itself and therefore caused no rejection. These now 'donor-friendly' T-cells then circulated within the recipient mouse's blood, Zavazava explained.
"When we then transplanted into the recipient mouse a donor mouse heart that had the same genetic make-up as the previously injected stem cells, the T-cells didn't reject the heart because they recognized it as compatible," Zavazava said.
"If we could eventually use this approach for organ transplantation in humans, it would be a huge advantage over the method we're currently using," he added.
In addition to its potential for organ transplantation treatment, the embryonic stem cell-based method might also have implications for treating bone marrow diseases such as leukemia.
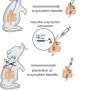
Because a mouse is so small, it was not possible in the study to remove the animal's existing heart and replace it with another. Thus, to test for transplant success, the study approach involved leaving the original heart intact, transplanting a second functional heart into the abdomen and then linking the transplanted heart to the aorta.
Source: University of Iowa