Metabolic insight to illuminate causes of iron imbalance
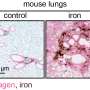
New insight into key players in iron metabolism has yielded a novel tool for distinguishing among root causes of iron overload or deficiency in humans, the researchers report in the August issue of Cell Metabolism, a publication of Cell Press. While the body needs iron to produce hemoglobin, a substance in red blood cells that enables them to carry oxygen, too much iron can build up and eventually damage organs.
The balance of iron in mammals is controlled by a liver-produced hormone called hepcidin and the iron transporting receptor ferroportin, researchers knew. Hepcidin binds ferroportin to stimulate its break down, thereby lowering iron export. Too much hepcidin results in anemia; too little and the body doesn't rid itself of enough iron. (The most common human disease of iron overload is hereditary hemochromotosis, which affects about five out of 1000 Caucasians in the U.S., according to the National Institutes of Health.)
Now, researchers have identified the critical hepcidin-binding domain (HBD) on ferroportin. By placing that binding site on a bead, they now have a very specific method for detecting hepcidin levels in human blood.
"We've identified the hepcidin-binding site," said Jerry Kaplan of the University of Utah, Salt Lake City. "It will allow the diagnosis of underlying inflammation to distinguish diseases of iron metabolism that stem from hepcidin versus those with other causes."
Hepcidin was first known not for its effects on iron but for its antimicrobial action, explained Kaplan and his colleague Diane Ward, also of the University of Utah. The liver produces more of the hormone in response to inflammatory cytokines as a defense mechanism. Because microorganisms need iron, increases in hepcidin that lead to a decline in ferroportin and iron are believed to be antimicrobial, he explained.
In addition to zeroing in on the hepcidin-binding site in the new study, Kaplan and Ward showed that their HBD assay can readily detect variations in serum hepcidin levels due to mutations in genes known to affect hepcidin levels as well as mutations in other genes involved in iron metabolism.
While other tests for hepicidin have been developed, the new assay is unique in that it specifically identifies the hormone's biologically active form. Due to the remarkable degree of evolutionary conservation of the binding site, the new assay could also be used in other vertebrates, from cows to fish, they said.
" This test narrows it down to [active hepcidin]," Ward added. "It can help us divine the effects of inflammation on body iron stores."
The researchers made another unexpected discovery. Human hepcidin binds ferroportin at 37? Celsius, but not at 4?. The reason, they show, is that the hepcidin from humans changes its conformation at low temperatures.
Most mammals never get that cold, so the physiological relevance wasn't clear. But, the researchers wondered what it might mean for other, cold-blooded vertebrates like fish that can live in very cold waters.
They found that the hepcidin of zebrafish continued to bind at low temperatures, despite the fact that the hepcidin-binding domain of the fish was nearly identical to that from humans. The same was true of brown trout collected in the middle of the Utah winter, along with Alaskan nine-spine sticklebacks and a frog, they show. The difference between mammals and the fish seems to lie in a portion of the hepcidin structure outside of the binding domain.
Their studies led to another evolutionary insight. Most mammals have just one hepcidin gene, but fish have multiple, earlier studies had shown. One of the fish hepcidins is a full-length, "mature" hepcidin, while the others are smaller versions. They now show that the full-length hepcidin of fish has little antimicrobial power against E. coli. Together with earlier evidence, the result suggest that mammalian hepcidin has both iron regulatory and antimicrobial activity, while fish hepcidin genes have evolved to separate these two functions, they said.
Source: Cell Press