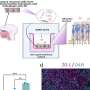
Immune exhaustion in HIV infection
As HIV disease progresses in a person infected with the HIV virus, a group of cells in the immune system, the CD8+ T lymphocytes, become “exhausted,” losing many of their abilities to kill other cells infected by the virus. For many years scientists have debated whether this exhaustion of CD8+ T cells is the cause, or the consequence, of persistence of the HIV virus. In a study published this week in PLoS Medicine, Marcus Altfeld and colleagues studied the immune response over time amongst 18 individuals who had very recently become infected with HIV.
These researchers found that the presence of high amounts of HIV in the blood seemed to cause CD8+ T cell exhaustion; when antigen was reduced, either as a result of treatment with antiretroviral drugs, or evolution of viral epitopes to avoid recognition by CD8+ T cells, these epitope-specific CD8+ T cells recovered some of their original functions. These findings suggest that CD8+ T cell exhaustion is the consequence, rather than the cause, of persistent replication of HIV.
In a related article, Sarah Rowland-Jones and Thushan de Silva (from the Medical Research Council in Gambia), who were not involved in the study, discuss approaches to treat HIV efficiently by suppressing the viral load early in infection aimed at preserving HIV-1-specific immune function. They evaluate whether such strategies are likely to be practical.
Citation: Streeck H, Brumme ZL, Anastario M, Cohen KW, Jolin JS, et al. (2008) Antigen load and viral sequence diversification determine the functional profile of HIV-1– specific CD8þ T cells. PLoS Med 5(5):e100. medicine.plosjournals.org/perl … journal.pmed.0050100
Source: Public Library of Science