Study shows how 'horse tranquiliser' stops depression
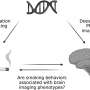
Researchers have shown exactly how the anaesthetic ketamine helps depression with images that show the orbitofrontal cortex – the part of the brain that is overactive in depression – being ‘switched off’.
Ketamine, an anaesthetic that is popular with doctors on the battlefield and also with vets because it allows a degree of awareness without pain, is a new hope for the treatment of depression – but the minute-by-minute images produced by Professor Bill Deakin and his team show how the drug achieves this in an unexpected way.
The drug deactivates the orbitofrontal cortex – located above the eyes, in the centre – which is thought to give rise to highly emotional thoughts such as guilt and feelings of worthlessness and causes reactions in visceral body parts such as a churning stomach and a racing heart.
Professor Deakin, of the Faculty of Medical and Human Sciences, said: “We were surprised to see it working on that part of the brain. We expected to see it work on the parts that control psychosis, at the sides of the brain. There was some activity there but more striking was the switching off of the depression centre.”
The study, published in the Archives of General Psychiatry, sought to identify the sites of action of ketamine but also the release of glutamate turned out to be important in ketamine’s effects and this could point to new quick treatments to get people out of severe or long-standing depression.
The team at the University’s Neuroscience and Psychiatry Unit (NPU) and Imaging Science and Biomedical Engineering (ISBE) gave intravenous ketamine to 33 healthy male, right-handed volunteers at the Wellcome Trust Clinical Research Facility (WTCRF). Scans showed activity in the orbitofrontal cortex stopped immediately.
In studies in the US, depressed people found that their symptoms begin to improve 24 hours after taking ketamine and continued to improve for two days after that. Professor Deakin is now funded to develop this approach to treatment in psychiatric patients in the new £30M Biomedical Research Centre awarded to Central Manchester and Manchester Children’s Hospital NHS Trust just last month. He hopes to develop a treatment within the next five years.
He said: “The study results have given us a completely novel way of treating depression and a new avenue of understanding depression.”
Professor Helen Mayberg, at Emory University in the United States, who pioneered deep brain stimulation to stop overactivity of the orbitofrontal cortex, in which electrodes are used during brain surgery, agreed: “This is a terrific finding...of extreme interest to our ongoing deep brain stimulation studies.”
Source: University of Manchester