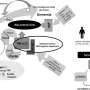
Scientists test device to track medication adherence in patients with HIV/AIDS
Most of us have missed a dose of antibiotic or forgotten to take a daily vitamin. But when the stakes are higher — as they are for people with HIV/AIDS — a skipped pill could mean the difference between health and hazard for the entire population.
Now, a breath monitoring device developed by scientists at the University of Florida and Xhale Inc. could help prevent the emergence of drug-resistant strains of HIV by monitoring medication adherence in high-risk individuals.
“For HIV, it’s been shown that if you don’t take a very high percentage of your medication, you may as well not take medication at all,” said Richard Melker, M.D., a professor of anesthesiology at the UF College of Medicine and chief technology officer for Xhale.
Patients who take some but not all of their medication increase the likelihood the virus will mutate into a deadlier, drug-resistant form. Experts have tried literally hundreds, if not thousands, of ways to monitor drug adherence, ranging from daily log books to blister packs that record the time each pill is dispensed. Despite the money, time and effort devoted to these methods, Melker said only one works well: directly observed therapy, or DOT.
“If you have a disease that is deemed to be a public health risk, authorities can put you into a program where you have to come to the clinic every day and be observed putting the pill into your mouth and swallowing it,” Melker said.
But that process is inconvenient for patients, as well as for clinic personnel who have to track them down when they fail to show up. A breath-monitoring device developed by UF scientists and Xhale could change that, allowing patients to participate in a type of virtual DOT from home.
“The machine sits in your home and when it’s time for you to take your medication, it makes a beeping noise. If you don’t hit a button after about five minutes, it’s going to beep louder and louder until you come,” Melker said. “If you don’t come after a certain amount of time, the machine can call the clinical trial coordinator and indicate that subject or patient didn’t take the medication as prescribed.”
The device, which is slightly smaller than a shoebox, records the results of each breath test, allowing patients to bring a memory card or USB key to the clinic once a month and receive a printout of their results. Eventually, the researchers hope to reduce the size of their detection device to fit inside a cell phone. But for now, they’re satisfied that the technology works.
“The doctor can see how often you took it and exactly what time. If it made the patient really sick or dizzy and they didn’t take it, they can find out why,” Melker said. “It’s not just a question of did I or didn’t I take it, but when you took it or why you didn’t take it.”
The researchers developed the adherence monitor by incorporating minute amounts of an alcohol into a gel capsule. The additive, called 2-butanol, is one of many GRAS — Generally Recognized as Safe — compounds approved by the Food and Drug Administration for use in foods.
“We wanted (patients) to swallow a chemical and have it transform into something else that’s easy to monitor,” said Matthew Booth, Ph.D., an assistant professor of anesthesiology at the UF College of Medicine and an investigator in the study. “When it hits the stomach lining and liver, an enzyme converts the alcohol to a gas that can be measured in the breath.”
To determine how well the byproduct could be detected, six healthy volunteers swallowed empty pills in which the capsules contained trace amounts of 2-butanol. After five to 10 minutes, the scientists could measure the volatile byproduct in the volunteers’ breath using a small detector. The scientists say their device could also be used to monitor medication adherence in patients with other communicable diseases, such as tuberculosis.
“It is encouraging that the biological and chemical elements of the adherence system work as predicted. We were able to conclusively show who swallowed the capsules containing the 2-butanol. With further optimization, we are optimistic the device will perform very well,” said Donn Dennis, M.D., the Joachim S. Gravenstein professor of anesthesiology at the UF College of Medicine and an investigator in the study.
The researchers say the device may prove equally helpful for monitoring adherence in clinical trials.
“If you enroll HIV/AIDS patients in a clinical trial and they don’t take the medication, then you may not get adequate proof that the drug is effective,” Melker said. “It might be effective, but some of the patients aren’t taking it.”
Phase 2 trials are often conducted in the community, rather than at research institutions, making it difficult for researchers to monitor adherence. As a result, many trials enroll a larger group of subjects than needed, in hopes they’ll obtain enough data to determine the safety and efficacy of the medication.
“If we had a good way of doing DOT that’s realistic, instead of having someone come to your house or you going to clinic every day of your life, then we would know whether these people stopped taking their medication and why. Right now, nobody knows any of that.” Melker said. “The implications of being able to understand what normal human behavior is in a clinical trial and, of course, in the real world, are huge.”
Source: University of Florida