Scientists studying sepsis in mice find potential drug targets for deadly disease
Scientists at The Scripps Research Institute have uncovered a connection between blood coagulation and the immune system that may have important implications for people with sepsis, a severe and difficult to treat disease that kills tens of thousands of Americans a year.
“We have identified a key connection of signaling pathways in the cascade of events leading to sepsis. This defines a crucial point where the immune system spirals out of control to cause severe sepsis and where there is an opportunity for therapeutic intervention,” says Scripps Research Professor Wolfram Ruf, who led the research with his postdoctoral fellow Frank Niessen. Their results are published in the February 27 advance, online issue of Nature.
Ruf and his colleagues identified a new cross talk involving the vascular coagulation system and certain cells in the immune system. By disrupting this cross talk, they were able to rescue mice from death due to sepsis. Though there is no guarantee this preclinical success will translate into human therapies, these proof-of-principle experiments may improve the diagnosis of heterogeneous sepsis syndromes and yield potent drugs for treating people who suffer from sepsis.
A Severe, Fast-Moving Disease
Sepsis is a severe, fast-moving, dramatic, and often fatal disease caused by an overwhelming bacterial infection that enters the bloodstream. These invading bacteria produce endotoxins and other toxic chemicals that trigger a widespread inflammatory response of the innate immune system—a response that is necessary, as it turns out, because without the inflammation, the body cannot fight off the bacterial infection.
Unfortunately, this inflammation can also spiral out of control leading to septic shock. During sepsis, the inflammation triggers widespread coagulation in the bloodstream. This coagulation can block blood vessels in vital organs, starving the organs of oxygen and damaging them. The organs can be further damaged when the blood starts to flow again because the lining of the blood vessels remain leaky due to inflammatory cytokines and damage by intravascular coagulation. This leads to edema, the buildup of liquid in tissues and allows immune cells to exit the bloodstream and enter the tissue. Inside the tissues, the immune cells can cause severe damage and organ failure. Frequently, the vital function of kidneys and lungs are affected.
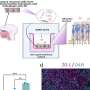
Sepsis syndrome can be either fulminant or protracted when patients are not able to cope with and to recover from severe infections. Overall, the prognosis for sepsis is dire. It is one of the leading causes of death for both infants and adults in the United States, and, according to the Centers for Disease Control and Prevention (CDC), it accounted for more than 33,000 deaths in 2004 alone—the last year for which complete statistics are available.
Numerous therapeutic approaches to treating sepsis have been tried through the years. For many years, the only option was to administer powerful, broad-spectrum antibiotics to control the bacterial infection. By the time these were administered, however, it was often too late. The antibiotics did not affect the existing bacterial toxins in the bloodstream, and they could not counter what appeared to be a self perpetuating inflammatory response that results from these toxins. Therapeutic approaches that attempt to reduce inflammation have proven to make people worse off than they were without treatment because those therapies compromise the immune response, unshackling the bacteria in the process.
Another possible approach to intervention involves exploiting the connection between coagulation and immunity, and anticoagulants have proven to be an effective treatment in severe sepsis. In recent years, the U.S. Food and Drug Administration (FDA) approved a recombinant form of activated protein C (Xigris) for treating sepsis, which is believed to work, in part, by controlling coagulation. However, other anticoagulants have failed in clinical trials and recent experiments in mice indicate that Xigris protects the vascular endothelium directly through cell signaling, rather than regulating coagulation.
A New View of Sepsis
The coagulation cascade is a tightly controlled mechanism designed primarily to prevent blood loss due to injury, but is also aberrantly activated in diseases like Ebola and sepsis. Though the link between coagulation and inflammation is one that scientists have known about for years, the exact molecules that connect coagulation to the inflammatory response in sepsis have remained a mystery. Ruf and his colleagues, wanting to understand the process, turned to knockout mice missing signaling receptors for coagulation enzymes, called the protease activated receptors (PARs).
Specifically, they found that mice lacking PAR1, also known as the thrombin receptor, were less likely to die from sepsis. Surprisingly, PAR1-deficient animals initially became very sick when exposed to endotoxin, but recovered more quickly from systemic inflammation and thereby escaped the deadly complication of sepsis syndrome. It turned out that normal mice could also be rescued from death when they received pharmacological drugs that block the PAR1 receptor or very high doses of coagulation inhibitors. This therapeutic intervention was successful, even when inflammation had already peaked. These experiments provided the first clue to indicate that it is the cell signaling component of the coagulation cascade that triggers severe systemic inflammatory response syndromes.
It was originally believed that coagulation in the blood stream damages endothelial cells that line the vasculature. This damage, in turn, helps activate platelets and leucocytes to cause thrombosis and organ damage. Ruf and his colleagues discovered that –unexpectedly—coagulation activates the immune system directly to promote sepsis syndrome. In particular, the dendritic cells of the mouse’s immune system play an important role and these cells are perturbed in the lymphatic system, rather than in the blood stream.
Typically dendritic cells produce potent pro-inflammatory cytokines in the lymph nodes during immune reactions. When the dendritic cells sense the increased coagulation in sepsis, they migrate faster through the lymphatic system and as a result do not stay put in the lymph nodes. This causes a release of inflammatory cytokines and chemical signals directly into the lymph. Lymphatic fluid is constantly recycled into the blood stream through the thoracic duct. This major lymph vessel connects to the blood stream immediately before blood enters the lungs. In sepsis, inflammatory mediators in the lymph fluid are thereby directly delivered to one of the most vital organs in the body.
In further research of this novel sepsis mechanism, Ruf and his colleagues uncovered downstream components of the PAR1 signaling pathway. Making use of chemical probes provided by the Scripps Molecular Screening Center, they identified that protease signaling on the dendritic cells induces the production of sphingosine 1 phosphate (S1P), a bioactive lipid that activates another G protein-couples receptor, the S1P receptor 3 (S1P3). In mice that lacked this receptor, they showed that dendritic cells are also responsible for triggering disseminated intravascular coagulation in sepsis. Through the connection between S1P3 and PAR1, dendritic cells are caught in an amplification circuit whereby they activate coagulation, and are in turn excited by one of the enzymes in the coagulation cascade to produce severe systemic inflammation.
Ruf and his colleagues showed that interrupting the S1P3 and PAR1 communication not only prevents the spread of inflammation though the body, but confines the inflammatory reaction to a desired location: the lymph node where the immune system fights microorganisms. This research provides a new view of sepsis and identifies potential targets that might restore a beneficial inflammatory response while blocking the deadly consequences of sepsis. The researchers are now evaluating which targets would be most amenable to clinical development and are testing the broader relevance of this pathway for other infectious diseases.
Source: Scripps Research Institute