Researchers identify cells that cause nervous system disease
Two teams of University of Michigan researchers have tracked down the cells responsible for neurofibromatosis type1, a disfiguring, incurable condition and one of the most common hereditary disorders.
"We now know what cells to target. And that's a big step toward new therapies," said Sean Morrison, director of the U-M Center for Stem Cell Biology and leader of one of the research teams. The other group was headed by Yuan Zhu of the U-M Medical School.
Neurofibromatosis type 1, or NF1, is a peripheral nervous system condition that afflicts one in 3,500 Americans. Symptoms normally begin to appear by age 10. Though most cases are mild, the disease can lead to disfigurement, learning disabilities, blindness, skeletal abnormalities, loss of limbs and, occasionally, lethal malignancies.
NF1 causes benign tumors to grow around peripheral nerves; in 3 to 5 percent of the cases, the tumors later become malignant. The most common NF1 tumors are called neurofibromas.
Researchers have long wondered which of the body's cell types triggers the formation of neurofibromas: Is it the Schwann cells, which form the protective myelin sheath around nerve fibers, or is the true culprit the stem cells that give rise to Schwann cells during fetal development? The answer has implications for the development of drug therapies.
The two U-M studies demonstrate that a special type of Schwann cell is likely to blame, not stem cells. Both reports will be published Feb. 5 in the journal Cancer Cell.
"People have increasingly focused on the link between stem cells and cancer," said Morrison, a U-M Life Sciences Institute researcher and a Howard Hughes Medical Institute investigator. "What we're saying here is that it's not always the stem cells. The mature cells, even in the nervous system, can give rise to these cancers."
In 1990 two teams—one led by former U-M geneticist Francis Collins—discovered that NF1 is caused by one enormous gene on chromosome 17. NF1 is the most common neurological disorder caused by a single gene.
The NF1 gene makes a large and complex protein called neurofibromin, which acts as a molecular brake to prevent nervous system cells from overmultiplying. A mutation to the NF1 gene can release that brake and set in motion the runaway freight train of uncontrolled cell division that results in tumors.
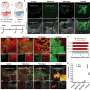
Over the years, Morrison's lab has developed specialized tools that allow researchers to track and study neural crest stem cells, which give rise to the peripheral nervous system—the vast network of nerves that branch out from the brain and spinal cord. Neural crest stem cells usually disappear before birth, once they've completed their mission.
In the current study, Morrison-lab scientists Nancy Joseph and Jack Mosher tried to determine if deleting the NF1 gene can somehow cause neural crest stem cells to persist beyond birth and form neurofibromas in mice.
The researchers studied seven mouse models that had various mutations of the NF1 gene and other genes known to contribute to the formation of neurofibromas and their cancerous counterparts, malignant peripheral nerve sheath tumors.
"The surprise was that we didn't see neural crest stem cells persist after birth in regions where the tumors formed, even with the NF1 deletions," Joseph said. "That argues against a stem cell origin."
The Morrison lab's study, when combined with work done in Zhu's lab, led U-M researchers to conclude that Schwann cells, not neural crest stem cells, proliferate to form the tumors.
In fact, Zhu and his colleagues were able to show that a specific type of Schwann cell, called a non-myelinating Schwann cell, is the likely source of potentially cancerous neurofibromas.
"One of the difficulties of NF1 is that it is hard to predict when tumors will grow and which tumors will turn malignant. You don't want to use a very aggressive therapy because some tumors will never grow," said Zhu, an assistant professor of molecular medicine and genetics at the U-M Medical School and a member of the U-M Comprehensive Cancer Center.
In addition to pinning down the cell type, Zhu's lab determined how non-myelinating Schwann cells start overmultiplying. They found that nerve damage and inflammation were among the two earliest events in tumor initiation.
"With this insight into the initiation of the disease, we can develop strategies to prevent the tumors from forming," Zhu said.
Source: University of Michigan