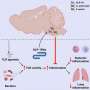
Jefferson neurosurgeons using new liquid treatment for wide-neck brain aneurysm
Neurological surgeons at Jefferson Hospital for Neuroscience are among the first surgeons in the United States using an FDA-approved liquid system for treating wide-necked brain aneurysms, which could eventually replace current treatments.
Principal investigator Erol Veznedaroglu, M.D., associate professor of Neurological Surgery and director of the division of Neurovascular Surgery and Endovascular Neurosurgery, Thomas Jefferson University Hospital, is one of the few surgeons selected to explore the use of a liquid embolic (blocking) system to fill wide-neck brain aneurysms, which have a wide opening where the aneurysm arises from the artery or blood vessel. A brain aneurysm is a weakness in a major blood vessel that causes a portion of the vessel wall to balloon out. This abnormality puts an individual at risk should the aneurysm break open and bleed.
“A wide-neck brain aneurysm is relatively uncommon and occurs in about 25 percent of persons with brain aneurysms,” said Dr. Veznedaroglu. “Wide-neck aneurysms can be difficult to treat both surgically (brain surgery to clip off the aneurysm) and endovascularly (treatment done from within the blood vessel), which are methods used to treat other types of brain aneurysms.”
“The potential benefit of the liquid embolic system may be the complete or partial blockage of the blood supply to the aneurysm,” said Deborah L. August, M.D., MPH,
director of Clinical Research in the department of Neurological Surgery, Jefferson. “It may also help to correct or lessen some symptoms.”
Current treatments for brain aneurysms include open brain surgery to clip the aneurysm
and coil embolization or coiling, less–invasive surgical procedure. For coiling, a catheter is inserted into an artery in the groin, then advanced into the affected artery in the brain.
X-rays are used to guide the catheter into the artery.
“Coils are the most commonly used embolization device but some wide-neck aneurysms have such a large opening that the coils may not stay inside the aneurysm sac,” said
Dr. Veznedaroglu. “In this case, the coils can fall back into the blood vessel and block or partly block the blood flow.”
Researchers noted they are not recruiting patients, as this is not a clinical study.
Rather, this is a Humanitarian Use Device which is used to diagnose or treat a disease or condition that affects fewer than 4,000 individuals in the United States per year and for which no comparable device is available.
The Food and Drug Administration (FDA) allows physicians to use such a device under a Humanitarian Device Exemption, when a device maker chooses not to do formal research studies to test a product as it would be used to treat a smaller population of patients.
“Before the FDA gave the exemption, it looked at facts given by the maker of the device and decided that the likely risks of using the system are within reason, compared to the possible benefits of using this device and compared to other treatments for a wide neck aneurysm,” said Dr. August. “Research studies have not been done to show whether this system works for treating wide-neck aneurysms.”
By filling the aneurysm sac or pocket with the liquid, blood flow into the aneurysm is blocked, helping to prevent the aneurysm from rupturing or increasing in size.
This treatment is done endovascularly and essentially consists of inserting a catheter into the blood vessel to cut off the blood supply. The material is delivered by slow-controlled injection through a very micro-size catheter into the aneurysm under x-ray visualization. The catheter is initially inserted into a vessel in the groin area and threaded to the vessel where the aneurysm is located. The material enters the aneurysm as a liquid through the catheter and then begins to solidify from the outside to the inside with final solidification or embolization occurring within five minutes.
To be eligible for such a procedure, a patient must 18 years or older, not have an intracranial stent and/or coils or severe liver or kidney disease. Women who are pregnant or nursing are also not eligible.
Source: Thomas Jefferson University