Mental health needs of soldiers increase several months after returning from Iraq war
Compared to initial screening upon returning from the Iraq war, U.S. soldiers report increased mental health concerns and needs several months after their return for problems such as posttraumatic stress disorder and depression, according to a study in the November 14 issue of JAMA.
“Our previous article described the Department of Defense’s (DoD) screening efforts to identify mental health concerns among soldiers and Marines as they return from Iraq and Afghanistan using the Post-Deployment Health Assessment (PDHA). However, the article also raised concerns that mental health problems might be missed because of the early timing of this screening. It cited preliminary data showing that soldiers were more likely to indicate mental health distress several months after return than upon their immediate return. Based on these preliminary data, the DoD initiated a second screening similar to the first, to occur 3 to 6 months after return from deployment,” the authors write.
Charles S. Milliken, M.D., of Walter Reed Army Institute of Research, U.S. Army Medical Research and Materiel Command, Silver Spring, Md., and colleagues analyzed the mental health responses of the first cohort of soldiers (n = 88,235) to complete both the initial screening and the new later screening, with a median (midpoint) of six months between the two assessments. Both screenings included a self-report questionnaire and a brief interview with a clinician.
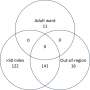
The researchers found that soldiers reported more mental health concerns, such as posttraumatic stress disorder (PTSD), major depression or alcohol misuse during the later screening. Of the 88,235 soldiers, 3,925 (4.4 percent) were referred for mental health care during the initial screening and 10,288 (11.7 percent) were referred during the later screening. Combined data from both screenings showed that the clinicians identified 20.3 percent of active and 42.4 percent of reserve soldiers as needing referral or already being under care for mental health problems.
Among active component soldiers, use of mental health services increased substantially following the later screening, especially within 30 days of the assessment. The majority of all soldiers who accessed mental health care (74 percent, n = 9,074) had not been identified as needing referral.
Concerns about interpersonal conflict increased 4-fold between the two screenings. Soldiers frequently reported alcohol concerns, yet very few were referred to alcohol treatment. Although soldiers were much more likely to report PTSD symptoms on the later screening instrument, 49 percent to 59 percent of those who had PTSD symptoms identified on the initial screen improved by the time they took the later screen, suggesting that the increase was due to new symptoms being reported.
“The study shows that the rates that we previously reported based on surveys taken immediately on return from deployment substantially underestimate the mental health burden,” the authors write. “This emphasizes the enormous opportunity for a better-resourced DoD mental health system to intervene early before soldiers leave active duty.”
“Increased relationship problems underscore shortcomings in services for family members. Reserve component soldiers who had returned to civilian status were referred at higher rates on the [later screening], which could reflect their concerns about their ongoing health coverage. Lack of confidentiality may deter soldiers with alcohol problems from accessing treatment. In the context of an overburdened system of care, the effectiveness of population mental health screening was difficult to ascertain.”
Source: JAMA and Archives Journals