Researchers discover method for identifying how cancer evades the immune system
One of the fundamental traits of a tumor – how it avoids the immune system – might become its greatest vulnerability, according to researchers from the University of Southern California. Their findings, demonstrated in human breast and colorectal cancers, indicate that a technique for determining a tumor’s “immune signature,” could be useful for diagnosing and treating specific cancers.
In the July 1 issue of Clinical Cancer Research, a publication of the American Association for Cancer Research, the researchers describe a means for determining which genes have been altered in a tumor to allow it to evade the body’s natural defenses. In time, the researchers believe such analysis could become a standard practice in cancer diagnosis and treatment.
“The implication is that once you know the mechanism by which tumors evade the immune system, you can match that tumor to available therapies,” said senior author Alan L.Epstein, M.D., Ph.D., professor of Pathology at USC’s Keck School of Medicine. “First, we find the genetic changes that allow a tumor to defeat the immune system, then we can apply therapies that compensate for these genetic alterations.”
According to Epstein, tumors are notorious for demonstrating a broad array of genetic and biological variations. Their differences vary widely between cancer types, even between subcategories within a particular type of cancer. However, while the genetic variations that comprise an immune signature are complex, the researchers discovered that a small subset of genes is integral in explaining immunological behavior.
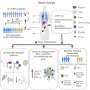
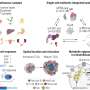
Using real-time PCR (rtPCR), a high-speed gene amplification technique, Epstein and his M.D./ Ph.D. student, Rebecca Sadun, screened tumors to identify 14 pro-immunity genes, which tumors downplay, and 11 key anti-immunity genes, which tumors promote. They studied the expression of these genes in five mouse tumor models for breast cancer, leukemia, colon cancer, lung cancer and renal cell carcinoma. They then compared two of these immune signatures with corresponding human tumors, eight cases of human ductal carcinoma and 11 cases of colorectal cancer.
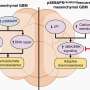
Remarkably, the researchers found that the immune signatures of each of the human breast cancer cases nearly matched that of mice. In all cases, the researchers saw a suppression of CD83 and CD28, two genes that affect activation of immune cells, and over-production of B7-H4, a gene whose protein product inhibits immune activation. The human colorectal cancers, however, showed variations in their immune signatures, which researchers saw as an indication of the need to understand the signature for each patient’s individual cancer.
“I see it as the beginning stages of personalized medicine, where we develop tactics for treating the unique genetic make-up of a specific tumor,” Epstein said. “It becomes even more necessary when we look at all the immunotherapies that are becoming available or are beginning to emerge from research.”
In time, Epstein believes, it will be possible to study the immune signatures for most, if not all, forms of cancer. In addition, rtPCR technology allows for a relatively inexpensive and rapid analysis on equipment available at most medical centers, researchers said. “For now, we need to better understand the immune signatures for the most common human cancers in order to identify the most important targets for immunotherapy,” Epstein said.
Source: American Association for Cancer Research