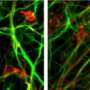
Scientists build Parkinson's disease in a dish to study cells' death
Until now, there have been no witnesses to the death of brain cells in people with Parkinson's disease. And like any murder mystery, this has slowed the search for the killer.
In a big break in the case, Stanford University scientists say they have re-enacted this tragedy in a petri dish - growing the young neurons from the donated skin cells of Parkinson's patient Genia Brin, the mother of Google co-founder Sergey Brin - and then watching them sicken and perish.
This feat, co-authored in last month's issue of the journal Cell by Stanford's Renee Reijo Pera, could accelerate the search for a cure of the crippling disorder. The research makes it possible, for the first time in medical history, to study the diseased cells and test compounds that might slow or even prevent their development.
"For the first time ever, we have them in a dish where we can study them directly. We can see exactly why they're dying, and test drugs in them," said Dr. William Langston of the Sunnyvale-based Parkinson's Institute, who contributed to the effort.
"I'm impressed, almost proud," said Brin, 62, of Los Altos Hills, Calif., who donated a dime-sized sample of skin cells, excised from her upper arm, which were taken to the Stanford lab and reprogrammed, using stem cell techniques, and turned into neurons, or brain cells. "It is a bad disease and its biological basis is little understood. Research has been pretty slow.
"I was hoping they would learn something from it," Brin said, "and they did."
Parkinson's disease, a degenerative disorder of the central nervous system, affects about 1 in every 250 people older than 40 and 1 in every 100 people older than 65. Among them are Intel founder Andy Grove and actor Michael J. Fox. In some, the disease progresses slowly; Brin, for instance, still skis and walks the Peninsula hills with her husband and dog. But in others, the quality of life can deteriorate dramatically, due to muscle rigidity, loss of balance and slow or uncontrollable movement.
It results from a death of cells in the brain that produce a chemical messenger called dopamine, which coordinates movement.
Most forms of the disease are not genetic. But there is one particular mutation of the LRRK2 gene that, while rare even among people with the disease, accounts for a substantial proportion of familial Parkinson's disease, especially among Ashkenazi Jews and other ethnic groups.
The mutation was detected in Genia Brin using a test made by the company 23andMe, co-founded by her daughter-in-law Anne Wojcicki. Brin had experienced mild symptoms, and knew her aunt had been sick.
"So I wasn't surprised to find out I had it. I was surprised that I had a double copy," meaning she had inherited the mutation from both parents. The 23andMe test showed son Sergey, 37, carried a single copy.
"The exact implications of this are not entirely clear," the Google co-founder wrote in a 2008 blog post. "Nevertheless, it is clear that I have a markedly higher chance of developing Parkinson's in my lifetime than the average person," a risk he estimated to be from 20 to 80 percent.
The family has since become major contributors to research. In addition to Genia Brin's cell donation to the Stanford study, Sergey has contributed money and his DNA to a vast study by 23andMe that aims to collect 10,000 volunteers to learn more about the genetic underpinnings of the disease.
There are no cures because research has been very hard to do, for two specific reasons: Only humans get the disease, so laboratory animals aren't good models for testing. And it is impossible to extract cells from deep inside the brains of patients. By the time patients die, the brain cells are dead, too.
"It is a huge bottleneck to research," Langston said.
But a new technique has changed all that. By inserting certain genes into skin cells, scientists can turn back the clock, causing them to revert to "induced pluripotent stem (iPS) cells" - with embryonic-like traits. Then they are coaxed into becoming mature cells, such as neurons.
This "disease in a dish" technique holds promise for not just Parkinson's but a whole range of other disorders, including Type 1 diabetes, Huntington's disease, Down syndrome and muscular dystrophy. Stanford scientists have even used the technique to build small faulty hearts to better understand rhythm disorders.
Genia Brin, an applied mathematician and retired research scientist at NASA's Goddard Space Flight Center, was considered to be the perfect donor because she has the genetic form of the disease. Scientists reason that they would have a better chance of replicating the disorder with her cells, rather than the cells of someone with a more sporadic form of the disease.
While rare, her form of the disease behaves just like the more common form, so it might offer important lessons.
But how long would it take her cells to sicken in the petri dish? No one knew. Research into the diseases of aging is challenging, because it is impractical to wait for decades for an ailment to develop.
"There was a good chance that a disease you get when you're 30 to 80 years old might not appear in 30 to 60 days in a dish," Langston said.
Initially, the cells acted normally, secreting dopamine and generating electrical signals.
But when they were subjected to toxic chemicals and stress, they began to act just like decades-old cells, churning out elevated levels of proteins that acquired aberrant three-dimensional shapes. This is thought to cause Parkinson's symptoms by clogging the cells, killing them, and halting critical dopamine production.
"We see them die. They no longer attach to each other, and spread out. They just float off," said Reijo Pera, director of Stanford's Center for Human Embryonic Stem Cell Research.
The next goal is to test compounds on the diseased cells that could someday be turned into medicines.
"Now that we can see that these neurons exhibit some of the earliest signs of the disorder," Reijo Pera said, "we can begin to develop methods to screen for factors that might protect them."
There are concerns that the iPS cells are not truly equivalent to embryonic stem cells, so researchers could discover differences in the mature neurons that are caused not by the disease, but by the process of making iPS cells.
And there's no guarantee that a treatment that helps this rare genetic form of the disease would also help the more common form.
But any clues, no matter how small, would be welcomed by those hunting this mysterious killer.
"Finding something to help these 1.5 percent of patients would be very nice," Langston said. "Finding something to help everyone - that would be huge."
"Now they can experiment with them," Brin said. "It was my cells that served this great purpose."
"I am not really hoping for a cure for myself in my lifetime," she said. "But I am hopeful for the next generation. " ... For Sergey and his children, and everyone else who has been touched by Parkinson's disease."
(c) 2011, San Jose Mercury News (San Jose, Calif.).
Distributed by McClatchy-Tribune Information Services.