Doctors treat adults' childhood heart defects
(PhysOrg.com) -- As director of the Adult Congenital Heart Disease clinic at Stanford, Daniel Murphy, MD, performs a job unheard of a generation ago. He cares for grown-up patients with cardiac defects that were once lethal in early life.
“In the past, most babies born with congenital heart defects did not survive childhood,” Murphy said. “Now, many of these adults need specialized care. It wasn’t available before because the patient population didn’t exist.”
The change began in the 1990s, as the first young beneficiaries of modern cardiac surgical techniques reached maturity. Today, 1 million U.S. adults live with the aftermath of a congenital heart defect. Caring for this population — which includes 35,000 Northern Californians — is a growing challenge for cardiologists, one that pushes the bounds of both adult and pediatric medicine. Lucile Packard Children’s Hospital and Stanford Hospital & Clinics have embraced the problem together. Their joint Adult Congenital Heart Disease clinic, founded in 2002, now sees 700 patients a year.
Ensuring continuity of care for survivors of childhood heart defects is Murphy’s top priority. Most of these people feel normal — they’re healthy-seeming, intellectually capable, productive members of society. In many cases, after surgery in infancy or childhood, they grew up thinking their hearts were permanently fixed.
“That’s a dangerous mistake,” Murphy said.
Some patients have not seen a cardiologist since childhood. Others may be seeking care, but face a communication and knowledge gap — doctors are only now learning to treat such problems in adult patients.
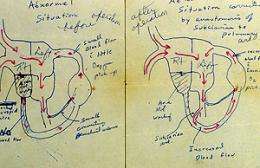
One middle-aged woman whom Murphy treated had developed an unusual way to bring physicians up to speed, he recalled. Whenever she needed to explain her heart condition, she would pull from her purse a yellowed diagram drawn by her pediatric heart surgeon decades before. The diagram showed her heart before and after surgical repair, and the patient had held onto it throughout her life.
“She understood her heart physiology better than many of the physicians who had taken care of her over the years,” Murphy said.
Follow-up with a knowledgeable caregiver is necessary because even patients who had simple cardiac problems in childhood may experience severe complications later, he said. Patients’ life expectancy is limited by problems that develop as a surgically repaired heart ages.
For example, heart valves that have been repaired or replaced may eventually become narrowed or leak. That places a silent burden on the heart. If it goes unnoticed too long, the resulting heart-muscle damage turns into heart failure, heart rhythm problems or sudden death.
“With surveillance, we can identify changes before they become life-threatening or permanent,” Murphy said.
In addition to providing regular monitoring, Murphy’s team helps patients navigate medical challenges such as pregnancy.
“Many women we see at the clinic were told they would never be able to have children,” he said. “We now know that’s not true for most, but they need planning and support.” Pregnancy and delivery place extra stress on the cardiopulmonary system, so it is important that pregnant women with unusual cardiac physiology receive care from an experienced, multidisciplinary team.
Packard Children’s high-risk obstetrics and maternal-fetal medicine practitioners frequently collaborate with Murphy to see patients through pregnancy, birth and the postpartum period.
“It’s one of the most gratifying aspects of what we do,” he said.
The clinic also conducts research on long-term consequences of different cardiac repairs. Studies of the current generation of adults are informing how pediatric cardiologists treat infants born today with congenital heart defects.
Murphy recommends that teens with congenital heart problems have an assessment when they are transitioning into adult care, so that they can get a clear view of their situation. The same holds true for adults with repaired congenital defects who have not had such an appointment with a specialty clinic.
“Patients deserve to know: what are my risks; where am I headed,’” Murphy said. “And they should have a point of contact for the future.”