Immune interaction optimises foetal nourishment during pregnancy
(PhysOrg.com) -- Paternal genes advise maternal immune cells on how to build the best womb for developing foetuses.
Researchers at the University of Cambridge and the Babraham Institute have identified a mechanism by which specific combinations of genes can lead to miscarriage and other complications in pregnancies.
The research revealed that paternal immune genes (MHC) in the placenta provide information to uterine natural killer (NK) cells to ensure that the foetus receives sufficient blood supply. Unlike their blood counterpart NK cells, which kill infectious and cancerous cells, uterine NK (uNK) cells actually help placental cells adapt the blood vessels in the womb to nourish the foetus.
By mating mice whose only genetic difference was in the MHC genes of the mother and father (1% of the genome), the researchers found that uNK cells would sense the difference in highly variable MHC genes. When faced with mismatched MHC genes from the father's immune system, uNKs were presumably not switched off and could focus on optimising the blood flow of the womb.
Francesco Colucci of the University of Cambridge Department of Obstetrics and Gynaecology had previously identified the particular genes expressed by mouse uNK cells and Ashley Moffett of the University of Cambridge's Department of Pathology had pioneered the research relevant to human uNK cells and MHC genes. But up until now, it was not clear which paternal MHC genes were expressed by mouse placentae.
"What is most exciting," Colucci says, "is that by revealing the similarities between human and mouse immunology of pregnancy, the [teams] lay new foundation for using mouse genetics to test new ideas and hypotheses informed by human genetics data."
The interaction of MHC and NK genes is also key in foetal programming of adult diseases such as diabetes and hypertension which are known to have early developmental origins
Colucci's work, published in Proceedings of the National Academy of Sciences of the United States of America (PNAS) yesterday, was funded by the BBSRC and the Wellcome Trust, along with the Centre for Trophoblast Research, Medical Research Council, and NIHR Cambridge Biomedical Research Centre.
Colucci describes the next steps of where this research is leading, saying, "We are now well positioned to explore how the inherent variability of these immune system genes affects reproductive success by comparing NK receptors and MHC in normal pregnancy to those with disorders."
In the future research, the 'good' and 'bad' combinations in humans will be mimicked in mice to examine uterine blood vessels and foetus/placenta growth. The results of these experiments should help provide an understanding of how to prevent pregnancy disorders.
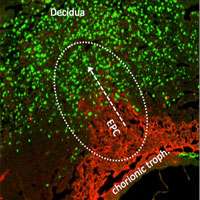
"This paradox has puzzled scientists for decades and understanding how the foetus evades rejection, except in severe pregnancy complications, has remained elusive," said Dr Myriam Hemberger of the Babraham Institute, the senior co-author who is an expert in mouse placental development. "Our findings show that paternal antigens on foetal trophoblast cells, which form the placenta and are therefore in direct contact with maternal tissue, help to transform the uterus for robust placental and foetal growth. This is essential for reproductive success."














