Study shows that delivering stem cells improves repair of major bone injuries in rats
(PhysOrg.com) -- A study published this week reinforces the potential value of stem cells in repairing major injuries involving the loss of bone structure.
The study shows that delivering stem cells on a polymer scaffold to treat large areas of missing bone leads to improved bone formation and better mechanical properties compared to treatment with the scaffold alone. This type of therapeutic treatment could be a potential alternative to bone grafting operations.
"Massive bone injuries are among the most challenging problems that orthopedic surgeons face, and they are commonly seen as a result of accidents as well as in soldiers returning from war," said the study's lead author Robert Guldberg, a professor in Georgia Tech's Woodruff School of Mechanical Engineering. "This study shows that there is promise in treating these injuries by delivering stem cells to the injury site. These are injuries that would not heal without significant medical intervention."
Details of the research were published in the early edition of the journal Proceedings of the National Academy of Sciences on January 11, 2010. This work was funded by the National Institutes of Health and the National Science Foundation.
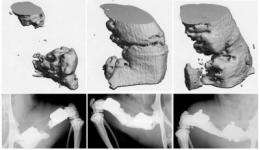
The study was conducted in rats in which two bone gaps eight millimeters in length were created to simulate massive injuries. One gap was treated with a polymer scaffold seeded with stem cells and the other with scaffold only. The results showed that injuries treated with the stem cell scaffolds showed significantly more bone growth than injuries treated with scaffolds only.
Guldberg and mechanical engineering graduate student Kenneth Dupont experimented with scaffolds containing two different types of human stem cells -- bone marrow-derived mesenchymal adult stem cells and amniotic fluid fetal stem cells.
"We were able to directly evaluate the therapeutic potential of human stem cells to repair large bone defects by implanting them into rats with a reduced immune system," explained Guldberg, who is also the director of the Petit Institute for Bioengineering and Bioscience at Georgia Tech.
Micro-CT measurements showed no significant differences in bone regeneration between the two stem cell groups. However, combining the two types of stem cells produced significantly higher bone volume and strength compared to scaffolds without cellular augmentation.
Although stem cell delivery significantly enhanced bone growth and biomechanical properties, it was not able to consistently repair the injury. Eight weeks after the treatment, new bone bridged the gaps in four of nine defects treated with scaffolds seeded with adult stem cells, one of nine defects treated with scaffolds seeded with fetal stem cells, and none of the defects treated with the scaffold alone.
"We thought that the functional regeneration of the bone defects may have been limited by stem cells migrating away from the injury site, so we decided to investigate the fate and distribution of the delivered cells," said Guldberg.
To do this, Guldberg labeled stem cells with fluorescent quantum dots -- nanometer-scale particles that emit light when excited by near-infrared radiation -- to track the distribution of stem cells after delivery on the scaffolds and completed the same experiments as previously described.
Throughout the entire study, the researchers observed significant fluorescence at the stem cell scaffold sites. However, beginning seven to 10 days after treatment, signals appeared at the scaffold-only sites. Additional analysis with immunostaining revealed that the quantum dots present at the scaffold-only sites were contained in inflammatory cells called macrophages that had taken up quantum dots released from dead stem cells.

"While our overall study shows that stem cell therapy has a lot of promise for treating massive bone defects, this experiment shows that we still need to develop an improved way of delivering the stem cells so that they stay alive longer and thus remain at the injury site longer," explained Guldberg.
The researchers also found that the quantum dots diminished the function of the transplanted stem cells and thus their therapeutic effect. When the stem cells were labeled with quantum dots, the results showed a failure to enhance bone formation or bridge defects. However, the same low concentration of quantum dots did not affect cell viability or the ability of the stem cells to become bone cells in laboratory studies.
"Although in vitro laboratory studies remain important, this work provides further evidence that well-characterized in vivo models are necessary to test the ability of regenerative tissue strategies to effectively integrate and restore function in complex living organisms," added Guldberg. "Improved methods of non-invasive cell tracking that do not alter cell function in vivo are needed to optimize stem cell delivery strategies and compare the effectiveness of different stem cell sources for tissue regeneration."
Guldberg is currently exploring alternative cell tracking methods, such as genetically modifying the stem cells to express green fluorescent protein and/or other luminescent enzymes such as luciferase. He is also investigating the addition of programming cues to the scaffold that will direct the stem cells to differentiate into bone cells. These signals may be particularly effective for fetal stem cells, which are believed to be more primitive than adult stem cells, according to Guldberg.
Lessons learned from the current work are also being applied to develop effective stem cell therapies for severe composite injuries to multiple tissues including bone, nerve, vasculature and muscle. This follow-on work is being conducted in the Georgia Tech Center for Advanced Bioengineering for Soldier Survivability in collaboration with Ravi Bellamkonda and Barbara Boyan, professors in the Wallace H. Coulter Department of Biomedical Engineering at Georgia Tech and Emory University.















