Scientists develop a new strategy to fight obesity
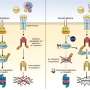
The antibody works against the gastric hormone ghrelin (pronounced "grell-in"), which has been linked to weight gain and fat storage through its metabolic actions. These findings point towards a potentially novel treatment for obesity that would interfere directly with the some of the biological mechanisms determining weight.
The study is being published the week of October 27, 2008, in an advance, online Early Edition of the journal Proceedings of the National Academy of Sciences (PNAS).
In the study, which was led by investigators Kim Janda and Eric P. Zorrilla of The Scripps Research, the antibody catalyst GHR-11E11 led to a higher metabolic rate in fasting mice and suppressed feeding following 24-hour food deprivation.
"Our study showed that this novel catalytic ghrelin antibody could specifically seek out and degrade ghrelin," said Janda, who is Ely R. Callaway, Jr. Professor of Chemistry, member of The Skaggs Institute for Chemical Biology, and director, Worm Institute of Research and Medicine (WIRM), at Scripps Research. "While this antibody lacks a high level of catalytic efficiency, our study clearly demonstrates that even a basal level of catalysis can effectively modulate feeding behavior. These findings not only validate antibody-based therapeutics, but strongly suggest that catalytic anti-ghrelin antibodies might help patients reach and maintain their weight loss goals."
According to recent reports from the World Health Organization, about 1 billion people worldwide are overweight or obese, with most of these in the developed world. In the United States, for example, the National Health and Nutrition Examination Survey found that, in 2003-2004, approximately 66 percent of all adults 20 years of age or older were overweight or obese. Almost four out of every five American men aged 40 to 59 were classified as overweight, according to a 2006 study published by the Journal of the American Medical Association.
Targeting Ghrelin
While non-surgical treatments can be modestly effective against obesity, weight loss or gain can be affected by ghrelin, which is released by the body to encourage eating during periods of calorie restriction. A gastric endocrine hormone produced primarily in the stomach, ghrelin promotes weight gain and fat storage through its metabolic actions, decreasing the break down of stored fat for energy as well as energy expenditure itself.
During periods of weight loss, the body produces high levels of ghrelin to encourage eating. Human studies have shown that ghrelin levels rise before meals and fall afterwards, findings that are consistent with the hormone's role in hunger and eating initiation. Indeed, circulating ghrelin levels are increased by food deprivation and decreased by eating, glucose load, insulin, and somatostatin, an important neural signaling hormone. Recent studies suggest mice deficient for ghrelin or its receptor store less of their consumed food and are resistant to diet-induced obesity. Also, small-molecule ghrelin receptor antagonists have been shown to reduce food intake, promote selective weight loss in the form of body fat, and improve glucose tolerance by augmenting glucose-induced insulin secretion.
The new study suggests the possibility that passive immunopharmacotherapy with a catalytic anti-ghrelin antibody such as GHR-11E11 could decrease the level of serum ghrelin as well as modulate energy homeostasis.
"The reason we looked at passive immunopharmacotherapy to treat obesity was because agonist/antagonist types of drugs have been remarkably unsuccessful," Janda said. "They are effective only while treatment is maintained and when treatment stops, weight returns. For obesity treatments to work, they must affect food intake and energy expenditure or storage—which is what this new catalytic antibody does by degrading ghrelin. Some people have the idea that because ghrelin is an endogenous hormone there might be too many adverse side effects if you eliminate it, but there is new evidence that the body itself produces antibodies against ghrelin."
Immunotherapeutic approaches against ghrelin may hold certain advantages over small-molecule antagonist treatments. First, immunoneutralization would occur outside the central nervous system, eliminating potential side effects that might occur with blood-brain barrier-penetrating small molecule antagonists. Second, therapeutic antibodies utilize the bloodstream as a site of action, which produces a pharmacological profile of safety and efficacy that is highly predictable and reproducible. In addition, immunization against a ligand may be more effective than small molecule receptor antagonist approaches when the receptor targets are unknown, multiple, or difficult to bind with any specificity.
Given the complex nature of obesity, any antibody-based strategy would most likely be used in combination with other available drugs, and as part of a comprehensive treatment approach that included nutritional, exercise, educational, and psychosocial components, Janda said.
However, he added, more research is needed. In addition to the development of more effective ghrelin antibodies, scientists need to better understand issues such as the effect of the antibodies over the long-term and their impact on individuals with varying body weights.
Source: Scripps Research Institute