When healing turns to scarring: Research reveals why it happens and how to stop it
For the first time, research from The University of Western Ontario has revealed the mechanisms involved in the origin of scarring or fibrotic diseases, as well as a way to control it. The study, led by Andrew Leask of the CIHR Group in Skeletal Development and Remodeling, is published in the Journal of Clinical Investigation.
"People are generally unaware of how prevalent scarring diseases are, and the impact they have on our health," says Leask, a professor in the Department of Physiology and Pharmacology at Western's Schulich School of Medicine & Dentistry. "Cardiovascular and other diseases including diabetes, cancer, and pulmonary fibrosis all involve scarring, which affects the organs' ability to function. Another example is scleroderma, a progressive scarring disease affecting 300,000 people in the United States and 40,000 Canadians. It's estimated about 40% of all deaths and health care costs in North America are related to scarring or fibrosis."
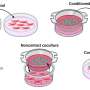
During tissue repair, specialized cells called myofibroblasts migrate to the wound where they generate the adhesive and tensile forces required for wound closure. Normally, these myofibroblasts then disappear from the wound. But if they persist and continue to make connective tissue, it can become too thick, preventing the organ from functioning properly. So for instance, in the case of diabetes, this scarring could cause the kidney to shut down, requiring dialysis or a transplant.
The research team which included investigators from Mount Sinai Hospital in Toronto and University College London in England, identified that a particular protein called glycogen synthase kinase 3 normally acts as a brake to terminate repair. If this protein is impaired, scarring results after wounding. Investigators also found elevated levels of a protein called endothelin-1. Next, they used a drug, already on the market, which blocks endothelin-1 and found it prevented scarring but did not affect wound closure in mice. While the use of the drug for this purpose would still have to be tested in humans, Leask believes this therapy could stop fibrosis from occurring without affecting normal tissue repair.
Source: University of Western Ontario