More aortic chest aneurysms being treated with less-invasive stents
An estimated 60,000 Americans are walking around with time bombs in their chests called thoracic aortic aneurysms. At any time, their main chest artery could suddenly burst open, causing massive internal bleeding that is almost always fatal.
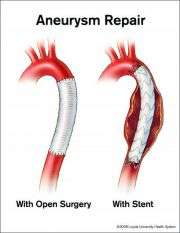
It's possible to repair the defect before the artery bursts, but traditional surgery is highly invasive. The operation typically requires an 18-inch incision, a week or two in the hospital and three to six months to recover. There are several major risks, including stroke and paralysis.
At Loyola University Hospital, an increasing number of patients are being treated with a device called a stent graft, which is inserted without opening the chest. Stent graft patients typically go home in a day or two, and recover fully in about two weeks.
At Loyola's Thoracic Aortic Disease Clinic, about 70 percent of patients who undergo surgery for aneurysms in the chest artery are receiving stent grafts rather than open chest surgery. "And as the technology evolves, we will be doing more and more stenting," said Dr. Jeffrey Schwartz, associate professor in the Department of Thoracic and Cardiovascular Surgery at Loyola University Chicago Stritch School of Medicine.
The stent graft used in chest arteries is a polyester tube covered by metal webbing. It is delivered with a catheter (thin tube). The surgeon inserts the catheter in a groin artery, and guides it to the thoracic aorta (chest artery). Once the stent graft is deployed from the catheter, the device expands outward to the walls of the artery. Depending on the patient, the stent graft is roughly 1 inch to 2 inches wide and 4 to 8 inches long, said Dr. Michael Tuchek, who has conducted several clinical trials of aortic stent grafts. Tuchek is a clinical assistant professor in the Department of Thoracic and Cardiovascular Surgery at Stritch.
James Feehan of Bolingbrook, Ill. recently received a stent graft to repair a life-threatening aneurysm in his chest aorta. The aorta is the main artery from the heart. An aneurysm occurs when the walls of the aorta thin and balloon outward. As the bulge grows, there's an increasing risk the aorta could suddenly burst. Feehan had undergone four earlier open-chest surgeries to repair other defects in his aorta. By comparison, the stent graft procedure was "a walk in the park," he said.
Feehan, 78, probably could not have survived another open chest surgery, said Tuchek, who placed the stent graft. Now, thanks to the stent graft, "he can go home and see his grandkids," Tuchek said.
The first-generation thoracic aortic stent grafts were approved in 2005. Feehan recently became one of the first patients in the country to receive the latest-generation stent graft, called Talent. The new device will make it possible for significantly more patients to have stent graft repairs rather than open surgery, Tuchek said.
The difference between the older stent grafts and the new one "is kind of like the difference between a Model T and a Ferrari," Tuchek said.
In a study published recently in the Journal of Vascular Surgery, researchers compared 195 patients who received the new stent graft with 189 patients who underwent traditional open chest surgery. About 84 percent of the open chest surgery patients experienced major complications, compared with only 41 percent in the stent graft group. After 12 months, 11.6 percent of the open chest surgery patients had died of aneurysm-related causes, compared with 3.1 percent in the stent graft group. Tuchek is a co-author of the study, which was funded by the manufacturer of the stent graft.
Loyola's thoracic aortic disease clinic follows more than 1,000 patients. About 80 percent of the patients have aortic aneurysms. Other conditions treated at the clinic include aortic dissection (the inner layer of the aorta's artery wall splits open) and ulcerated plaques (irregular buildup of cholesterol and other deposits in the aortic walls).
Risk factors for aneurysms and other aortic defects include smoking, hardening of the arteries, diabetes, family history, high blood pressure and congenital disorders such as Marfan syndrome. Many people do not realize they have aneurysms until the bulges are detected on CT scans or MRIs.
Because aortic disease is relatively uncommon, many surgeons and cardiologists refer patients to specialty centers such as Loyola. Loyola's aortic clinic treats patients from Illinois, Indiana, Wisconsin, Michigan and Iowa. Patients have come from as far away as Florida and Arizona.
The clinic is a collaborative effort. Schwartz, for example, specializes in open chest surgery, while Tuchek has helped pioneer the use of thoracic aortic stent grafts.
"My vision is that patients with aortic disease receive comprehensive, multi-specialty care for this unique condition," Schwartz said.
Source: Loyola University