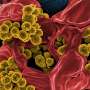
Patients who harbor the highly contagious bacterium causing staph infections can develop serious and sometimes deadly symptoms a year or longer after initial detection, a UC Irvine infectious disease researcher has found.
A study led by Dr. Susan Huang shows that almost one-quarter of the patients who acquire the antibiotic-resistant bacterium MRSA (Methicillin-resistant Staphylococcus aureus) developed staph infections at least a year after initial detection. The infections included pneumonia and blood diseases, some of which were linked to deaths.
The most serious staph infections begin in hospitals or other healthcare settings, such as nursing homes and dialysis centers. The study is the first to show such long-term risk of these infections and point to the need for new treatment approaches. Results appear in the July 15 issue of Clinical Infectious Diseases.
“Since infection risk remains substantial among long-term carriers of MRSA, these patients should be targeted for interventions along with patients who newly acquire MRSA,” said Huang, the epidemiology and infection prevention director at UC Irvine Medical Center.
Huang and Rupak Datta from Harvard Medical School followed 281 patients who had been MRSA-positive for anywhere from one to four years. Twenty-four percent developed invasive disease in the follow-up year, with pneumonia being the most common infection. MRSA was identified as a contributor to the deaths of 14 patients.
Staph infections can cause life-threatening skin infections, as well as infections in bones, joints, surgical wounds, heart valves and lungs. Older adults and people with weakened immune systems are at highest risk, although staph infections regularly occur in otherwise healthy people who are hospitalized.
MRSA is resistant to most antibiotics, but can be treated with vancomycin. Published studies show that approximately 2 percent of persons in the community and up to 5 percent to 8 percent of hospitalized patients harbor MRSA. The Centers for Disease Control and Prevention recommend that patients with MRSA be placed in single rooms and that medical staff wear gowns and gloves while caring for them to prevent spreading MRSA among patients.
“The severity of illness associated with MRSA in hospitalized patients urges us to identify the best way to reduce risks of infection,” Huang said. “Active research is ongoing to determine the safest and most effective intervention for different types of patients. Options include various antibiotic treatments, bathing agents and a hope for an effective vaccine.”
An assistant professor of medicine, Huang was an infectious diseases physician at Brigham & Women’s Hospital in Boston and an assistant professor at Harvard Medical School when the study was conducted. She joined UC Irvine in 2007.
Source: University of California, Irvine