Evidence found for genes that affect risk of developing Alzheimer's disease
Through one of the largest studies yet of Alzheimer’s disease (AD) patients and their brothers, sisters, and children, researchers at Mayo Clinic Jacksonville have found strong evidence that genes other than the well-known susceptibility risk factor APOE4 influence who is at risk for developing the neurodegenerative disease later in life.
Studying 25 multigenerational families of individuals diagnosed with late onset Alzheimer’s disease (LOAD), the most common form of the disorder, as well as hundreds of other participants, the research team found that blood levels of amyloid beta (Aß) proteins associated with AD were significantly elevated compared to protein found in non-blood relatives, such as spouses.
These first-degree relatives were cognitively normal and age 65 or less — many of them too young for symptoms of LOAD to show up.
“These results indicate that genetic factors of substantial magnitude lead to significant elevations of Aß in the blood of asymptomatic, young individuals from extended LOAD families,” says the study’s lead investigator, Nilufer Ertekin-Taner, M.D., Ph.D. “This fits with our hypothesis that A levels rise years before development of the disorder.”
The results, which first appeared online in October of last year, will be published in the Feb. 19 issue of Neurology.
The researchers have already identified three candidate genes on chromosome 10 that is associated with LOAD, and at least one of them, the gene that produces insulin degrading enzyme (IDE), is now regarded as a prime candidate for contributing to the disease. IDE degrades both insulin and amyloid protein, and scientists hypothesize that when there is too much insulin in the brain such as due to diabetes or lower expression levels of IDE, this may lead to toxic accumulation of Aß.
“We believe that 60 percent of the risk of developing the most common form of Alzheimer’s disease is genetic, and a good part of that is APOE4. But other genes are certainly contributing, and they could provide a platform for diagnosis and therapy in the future,” says the study’s senior author, Neill Graff-Radford, M.B.B.Ch., FRCP.
Dr. Ertekin-Taner estimates that the impact of these three genes could be as large as APOE4, which is a variant of the APOE gene that has been linked to LOAD. “Between 30 percent and 70 percent of AD can be attributable to APOE, and we estimate this locus of three genes on chromosome 10 could be as important,” she says. “The effect of the chromosome 10 locus could be due to multiple genes, with each gene having a smaller effect size than that of APOE.”
This study represents a decade of work by the Mayo researchers, who have been instrumental in discovering that one form of Aß known as Aß42 is much more toxic than the other common form of Aß, which is Aß40. They have also demonstrated that as AD progresses, Aß42 levels that have been rising for years begin to decline, presumably because more and more of the protein is being deposited within the brain.
Now, all known forms of early onset AD caused by genetic mutations are associated with an elevation of Aß42, and because there are such strong genetic determinants of these rarer forms of AD, the Mayo researchers speculated that the common late onset form may also be caused, in part, by genes that raise Aß levels.
In 2000, the team, led by Dr. Ertekin-Taner, published findings in Science magazine that targeted chromosome 10 as the site of some of these genes, whose function was unknown at the time. They had made the discovery by looking at 10 families of LOAD patients, and two other non-Mayo research teams published similar findings. The Neurology study is a continuation, and expansion, of that discovery.
This time, Mayo researchers collected data on 25 extended multigenerational LOAD families. In addition they studied 103 first-degree relatives of AD patients as well as a group of 116 participants in the federally-funded Mayo Clinic Study of Aging, who served as their comparison group. None of the study participants have been diagnosed with AD. They selected younger first-degree relatives and controls (age 20-65) to study so as to minimize the effect of age on Aß levels, and they also tested participants for their APOE variant. In a series of sub-studies in control groups, the investigators confirmed that blood Aß levels stayed consistent over a period of weeks, and that both Aß40 and Aß42 levels rise significantly in people over age 65 who do not have dementia.
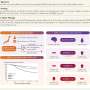
In the young, cognitively normal first-degree relatives of LOAD patients, they found that levels of both Aß40 and Aß42 in the blood were significantly elevated, compared to their spouses (which served as the control group). Studying the other group of 103 first-degree relatives of AD patients, the researchers also found significantly higher levels of Aß42.
Overall, comparing first-degree relatives with non-relatives, they found that for A42, the average level for the first-degree relatives is about 1.2–1.3 times that of non-relatives, and for A40, it was 1.1–1.4 times greater. Just like measuring cholesterol in the blood, the absolute magnitude of such an increase does not have to be large in order to be worrisome, Dr. Ertekin-Taner says.
They then determined that this rise in Aß is not due to the APOE4 gene. On the contrary, the plasma Aß levels of relatives with the APOE4 gene variant were lower — significantly so for Aß42 — than the levels of those who lacked the gene. This means two things, says co-author Steven Younkin, M.D., Ph.D.: that genetic factors other than the ones already known must lead to plasma A elevations in first-degree LOAD relatives, and that there is a strong mechanistic interaction between APOE4 and A leading to increased deposition of A in the brain and hence lower plasma A levels in these subjects.
“These findings indicate that there are genetic elevations in Aß levels in LOAD that cannot be explained by shared family environment,” Dr. Younkin says.
The results also suggest that “it is conceivable that plasma A, along with other information such as genetic variants, neuroimaging and cognitive test results, may be used in the future to identify individuals at risk for developing AD, before the onset of disease symptoms,” Dr. Ertekin-Taner says.
Source: Mayo Clinic