Receptor protein appears to be key in breakdown of kidney filtration
Massachusetts General Hospital (MGH) researchers have identified a new molecular pathway that appears to be involved in urinary protein loss (proteinuria). This early-stage kidney disease affects 100 million people around the world and is caused by a breakdown in the kidney’s filtering structures. Blocking this pathway could be a treatment for the condition and might significantly slow the process of kidney failure. The research team’s findings will appear in Nature Medicine and have been released online.
“We’ve identified a mechanism that underlies common forms of urinary protein loss and have data showing that it is operative in humans and in animal models of proteinuria,” says Jochen Reiser, MD, PhD, director of the Program in Glomerular Disease at the MGH Renal Division, the study’s senior author.
“Targeting this mechanism with antibodies or small molecule compounds can prevent or decrease proteinuria in animals, which may represent a novel therapy for kidney diseases such as diabetic nephropathy and focal segmental glomerulosclerosis,” adds Changli Wei, MD, PhD, first author of the article.
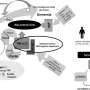
The kidney’s filtering activity takes place in clusters of blood vessels called glomeruli. Within those structures, extensions from cells called podocytes wrap around blood vessels. Tiny slits in the podocytes filter out excess water and waste materials, keeping larger proteins and blood cells inside the vessels. In several types of kidney disease, podocytes shrink and lose their structure, which compromises the filtering slits, allowing protein molecules to leak into the urine.
In the current study, the authors establish for the first time that the podocyte extensions called foot processes are capable of motion. In some kidney disorders, excess motility of these structures may be involved in the breakdown of podocytes that leads to proteinuria. To investigate this possibility, the researchers focused their attention on molecules known to be associated with cellular motility in a number of situations. One of these is the urokinase receptor (uPAR), which is known to be involved in wound healing and inflammation, as well as tumor invasion and metastasis.
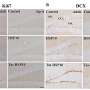
Reiser’s team found that uPAR expression is elevated in glomerular cells of patients with several forms of kidney disease, compared with healthy controls. Animal studies showed that uPAR is expressed in all glomerular cells, yet it does not appear to be required for normal kidney function, since renal function is not compromised in mice lacking the gene for the protein. When the uPAR-knockout mice were treated with a substance that usually induces proteinuria, they did not develop the condition, suggesting that the receptor’s presence is required for the breakdown of podocyte structure.
After the gene encoding uPAR was introduced into podocytes of the knockout mice, they began expressing the receptor within 24 hours and became susceptible to the proteinuria-inducing treatment. The researchers then showed that uPAR can associate with and activate another receptor protein, alphavbeta3 integrin, leading to podocyte motility. Blocking this step in the uPAR-controlled pathway could reduce or prevent the development of proteinuria in mice. Such an agent is currently in phase II clinical trials for the brain tumor glioblastoma and may become available for use in patients with proteinuria.
Further investigation is required to discover how the uPAR pathway may interact with other molecular mechanisms involved in proteinuria, including the activity of an enzyme called cathepsin L, reported earlier this year by members of the same research team. “We are working now in two directions – to better understand the relationship between uPAR and cathepsin L and to conduct a clinical trial with small molecules blocking uPAR or alphavbeta3 integrin,” says Reiser, an assistant professor of Medicine at Harvard Medical School. “We hope this could be the first step towards a cell-specific treatment of proteinuric kidney diseases that would add on to the great success of standard, but non-cell-specific interventions for these diseases.”
Source: Massachusetts General Hospital