T vs. B: Re-engineered human T cells effectively target and kill cancerous B cells
Human white blood cells, engineered to recognize other malignant immune cells, could provide a novel therapy for patients with highly lethal B cell cancers such as acute lymphoblastic leukemia (ALL), according to researchers at Memorial Sloan-Kettering Cancer Center (MSKCC). By administering repeated doses of T cells designed to express an artificial receptor which recognizes human B cells, the researchers were able to eradicate cancer in 44 percent of mice bearing human ALL tumors.
Their findings, published in the September 15 issue of Clinical Cancer Research, a journal of the American Association for Cancer Research, show that modified T cells – the white blood cells that actively fight infections – can be effective in fighting malignancies associated with B cells (immune cells that create antibodies) such as chronic lymphocytic leukaemia (CLL), ALL, non-Hodgkin's lymphoma (NHL). The researchers have an ongoing study using these T cells in CLL, and have recently begun the planning stages for a trial in patients with ALL.
“The immune system has evolved to police the body for infections and diseased cells, but it has a difficult time recognizing malignant cells since they largely appear normal to the immune system,” said lead study author, Renier J. Brentjens, M.D., Ph.D., medical oncologist in the Leukemia Service at MSKCC. “The idea is that we can take a patient’s own T cells, re-educate them by inserting a gene into them that will enable them to produce a receptor to recognize B cell cancers, and then return them to the patient where they should be able to attack and kill the tumor cells.”
Because the technique uses a patient’s own T cells, there is little risk of compatibility issues or rejection, as there might be with human stem cell transplant, Dr. Brentjens adds. Human stem cell transplant, following radiation or chemotherapy, is currently incorporated into the treatment of several B cell malignancies.
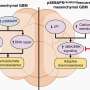
In order to get T cells to recognize B cells, Dr. Brentjens and his colleagues created a gene that encodes for a cell-surface protein – an artificial T cell receptor called a chimeric antigen receptor -- designed to specifically bind to CD19, a molecule found on the surface of B cells and B cell cancers. Antigen receptors are what allow T cells, in combination with other parts of the immune system, to recognize and attack infected or malignant cells. This chimeric gene, formed from active portions of several immune system-related genes, creates the chimeric antigen receptor protein called 19-28z, which does not require other co-stimulatory signals to fully activate T cells, according to Dr. Brentjens.
Dr. Brentjens and his colleagues used an engineered retrovirus to insert the chimeric antigen receptor gene into T cell DNA. Retroviruses insert DNA derived from their RNA into that of a host cell, which then uses viral vector-encoded genes to make specific proteins. In this case, the researchers infected healthy T cells with modified retroviruses containing the gene that codes for 19-28z. The T cell’s internal protein-making facilities then produce the chimeric receptor as if it were one of its own natural antigen receptors.
In Clinical Cancer Research, the MSKCC researchers detail the creation of 19-28z, their “second generation” chimeric antigen receptor, and its effectiveness in stimulating human T cells both in culture and in an animal model of human cancer. They also compared T cells engineered with 19-28z to T cells engineered with a “first generation” chimeric antigen receptor, lacking the co-stimulatory signal found in 19-28z. Their results showed that the “second generation” 19-28z receptor was superior to the “first generation” receptor, and that this T cell therapy works best when administered to mice through multiple weekly injections.
“The repeated boosts of new T cells during therapy to improve T cell persistence enhances the efficacy of these T cells in eradicating cancerous B cells,” said Dr. Brentjens. “This concept of T cell persistence being critical to treatment efficacy is one we are further investigating in current and upcoming clinical trials.”
The results have given the researchers further evidence that the technique will work in humans. When transplanted back into a patient, these engineered T cells could then attack and kill tumor cells bearing the CD19 protein. “CD19 is not found on the surface of bone marrow stem cells, so these modified T cells are reasonably safe since they should not attack other blood forming cells in the bone marrow following treatment,” Dr. Brentjens said.
Based on the results of their findings, the MSKCC researchers are currently conducting a clinical trial using this method in patients with chemotherapy-resistant CLL. CLL is currently considered an incurable cancer, Dr. Brentjens said, although the disease generally progresses slowly.
Source: American Association for Cancer Research