Aging stem cells in mice may hold answers to diseases of the aged
As stem cells in the blood grow older, genetic mutations accumulate that could be at the root of blood diseases that strike people as they age, according to work done in mice by researchers at the Stanford University School of Medicine.
"This and our previous work points out why older people are more likely to get blood diseases, such as leukemia or anemia, and are less likely to make new antibodies that would protect against infections like the flu," said senior author Irving Weissman, MD, director of the Stanford Institute for Stem Cell Biology and Regenerative Medicine and of the Stanford Comprehensive Cancer Center. The work will be published in the June 6 issue of Nature.
In past studies, this group of researchers had shown that blood-forming stem cells in the bone marrow of mice became less able to divide and replenish the supply of blood cells as they aged. The question was why.
Researchers have put forward many theories about how cells age, said Derrick Rossi, PhD, postdoctoral scholar and co-first author of the paper. One of those theories has to do with cells accumulating genetic mutations. "The idea is that, over time, accumulated DNA damage progressively diminishes the cell's ability to perform its normal function," he said.
However, researchers had thought that mutations were unlikely to underlie aging in blood-forming stem cells because they very rarely divide, and most mutations crop up during division. The infrequent divisions were believed to protect the cells from acquiring new mutations.
Rossi, Weissman and the other first author, postdoctoral scholar David Bryder, PhD, tested that idea in two different sets of experiments. In the first, they studied the blood-forming stem cells of mice engineered to have single mutations that make them especially prone to accumulating additional genetic errors. In each of the three different types of mutant mice they studied, the stem cells appeared to behave normally and to produce new blood cells.
However, the full truth came out when they took blood-forming stem cells from any of the three types of mice and used those cells to repopulate the bone marrow of irradiated mice. This type of experiment is much like using a bone marrow transplant to bring back the bone marrow in a person who has undergone extensive chemotherapy.
Normally, a few stem cells are enough to completely replenish the bone marrow of mice and produce normal amounts of blood and immune cells. However, error-filled blood-forming stem cells taken from the mutant mice were much less effective at colonizing the depleted bone marrow than normal stem cells, and became even less effective when taken from older mutant mice.
Rossi said these results suggest that mutations accumulating in stem cells as they age were preventing them from doing their normal job of producing new blood and immune system cells. However, these results were in mutant mice. Rossi wanted to know if the stem cells in normal, healthy mice also accumulate damage as they age.
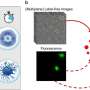
To address this, in the second set of experiments, Rossi isolated stem cells from the bone marrow of normal young and old mice, then stained those cells with a chemical that clings to a protein that's associated with DNA damage. This protein can act as a flag to highlight nearby DNA damage.
What he found is that young stem cells from normal mice contained no stain and therefore little or no DNA damage. Older stem cells, on the other hand, showed extensive staining.
All of this adds up to one thing: blood-forming stem cells do accumulate DNA damage with age even though they rarely divide, and that damage is passed on to the blood and immune system cells they make. Weissman said these findings could explain the origin of blood cancer (leukemia) and immune dysfunctions that occur as people age.
The next step is to show whether these results from mice hold true for human blood-forming stem cells. "If this work does extrapolate to humans, then it is absolutely consistent with the idea that blood-forming stem cells are the breeding ground for pre-leukemic mutations," said Weissman, the Virginia and D.K. Ludwig Professor for Clinical Investigation in Cancer Research.
Source: Stanford University Medical Center