Untangling a pathology of Alzheimer's
Researchers have uncovered what appears to be a natural protective mechanism against a central cause of neuronal death in Alzheimer's and similar neurodegenerative diseases. They theorize that it may be possible to use drugs to enhance that mechanism, to alleviate Alzheimer's pathology.
George Jackson, Daniel Geschwind, and their colleagues described their findings in the September 7, 2006, issue of the journal Neuron, published by Cell Press. Basically, in studies with mice, flies, and brain tissue from human patients, they discovered that the enzyme puromycin-sensitive aminopeptidase (PSA) snips apart the abnormal tangles of protein called tau that are associated with cognitive decline and neurodegeneration in Alzheimer's and similar "tauopathy" diseases.
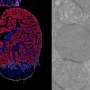
Significantly, they found higher levels of PSA gene expression in the cerebellum than in the cortex of patients with such diseases. The former region is known to be more resistant to neurodegeneration in such diseases than the latter. Tau causes neurodegeneration when a mutant form of the protein forms "neurofibrillary tangles" in brain cells, ultimately killing them.
In their experiments, Jackson, Geschwind, and their colleagues first used DNA microarrays--so-called "gene chips"--to find genes that were more activated in certain brain regions than others, in mice engineered to have a mutant form of human tau that causes neurodegeneration. Such microarrays enable researchers to determine the activity of thousands of genes at once. The gene for PSA was among those they identified as more active in the resistant cerebellum.
In studies with the fruit fly Drosophila, they found that higher activity of the PSA gene--and loss of its function--enhanced neurodegeneration. And in test tube studies, they found that PSA does directly act on tau to snip it apart for degradation by the cell.
They next compared levels of PSA gene expression in samples of brain tissue from the cortex and cerebellum of both normal humans and those with fibrillary tangle disorders. In both types of samples, they found a 5-fold elevation of PSA in the cerebellum as compared to the cortex.
The researchers concluded that their work not only reveals a significant protective factor in fibrillary tangle disorders, but points the way for further searches of other such factors. They wrote that "This work provides a clear proof of principle for validation of genetic screens using model systems and allows us to more firmly establish a functional role for one of the identified genes, Psa. Although Psa was known to be highly brain enriched, to our knowledge, its role vis-a-vis tau degradation or modification of tau-induced neurodegeneration has not been characterized previously.
"Data derived from in vivo studies with animal models and a cell-free system suggest that PSA may play a pivotal role in protection from tau-induced neurodegeneration, most likely by direct cleavage of tau," they wrote.
The researchers cited studies from other laboratories showing that turning off the mutant, pathological form of tau in mice after the mice showed neuronal pathology can reverse neurodegeneration. "Thus, it is tempting to speculate that factors that act to modulate tau levels or splicing, such as PSA, are candidates for playing a causal or contributory role in disease and may represent potential targets for development of therapeutics," concluded Jackson, Geschwind, and their colleagues.
Source: Cell Press