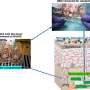
Finding the best therapy against bacterial infections is always challenging. Researchers from the Laboratory of Microfluidics and Complex Fluids, IPC PAS invented a microfluidic device which allows to test multiple antibiotics and antibiotic combinations at once. Credit: IPC PAS, Grzegorz Krzyzewski
Would you like to be able to find out which antibiotic combination works best for a particular patient? And do it in just six to 12 hours in a point-of-care? Or search for antibodies in thousands of samples at a time? This is now possible with a new device invented by scientists from IPC PAS. It is cheap, fast and reliable, and it can replace strip tests and give patients a better chance to fight disease.
A team led by prof. Piotr Garstecki is developing new tools for diagnostics. In a paper published in Micromachines, the describe combining existing simple methods to develop a simple bacterial susceptibility test kit that uses fewer reagents than a traditional test in agar, less antibiotics, and is as easy to perform as an Etest. Users can also choose how to visualize the results, selecting between metabolism indicators of the bacteria, fluorescent dyes or colorimetric change.
"We wanted to test antimicrobial susceptibility as simply as possible, not only for a single agent, but also for combinations or under different conditions," explains Dr. Ladislav Derzsi, one of the authors of the paper and supervisor of the project. "To deliver this new device, we matched several things that were discovered independently. For example, we used standard UV and soft lithography techniques which are very common methods to fabricate microfluidic devices and we combined it with non-contact printing on a machine that was designed especially for us."
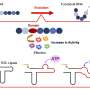
By using this combination of methods, the scientists could very precisely position small droplets of liquid in microwells—in this case, antibiotic solutions of different concentrations and in different combinations. They were printed inside microwells similarly to laser-jet or ink-jet printers. "Printers have small nozzles, and using piezoelectric forces, they deliver very precise amounts of liquid: nanoliters to picoliters, or even femtoliters," says Dr. Derzsi. "We use a similar technique, only instead of ink, we use antibiotics, and we inject them not on paper but onto a soft elastomer. We let it slowly dry out under controlled conditions. The aqueous phase—water—evaporates, and we're left with just the very small amount of antibiotic."
The wells used for the experiment were quite large—1 mm diameter—and their capacity was approx. 0.67 microliters. "In total, we're using 1024 wells in one chip. It is more than one order higher than classical plates with 96 wells despite being half the size. But it can be increased even to 10,000 wells by decreasing their individual size," says Dr. Derzsi.
To make it more user-friendly, the researchers bonded the device with a polymeric adhesive tape to seal it air-tight and then put it into vacuum. Thus, the device is delivered to the end user sterile and with inner negative pressure. "If we'd like to use it commercially, it could be additionally sealed in a vacuum bag [like we do with food items]," explains the scientist.
The user then has only to unpack it, inject a bacterial solution with a simple, commercially available pipette, and then add a small amount of oil that divides the wells and helps to avoid any cross-contamination between them. Then the whole pack is placed into the incubator. The growth or non-growth of bacteria indicates the optimal combination of antibiotics and their concentration.
A great advantage of the new testing system is its flexibility. It is possible to produce sterile plates on demand with different antibiotics in different combinations. Dr. Derzsi says, "We used plates with six single antibiotics in eight different concentrations and—to increase the precision—in eight repetitions each. We also tested pair-wise combinations of these six antibiotics in several repetitions. It is possible to test combinations of an arbitrary number of different antibiotics, inhibitors and adjuvants in one well, but usually, doctors don't use more than two at a time to avoid overburdening patient's system. By using this new method, doctors can test the patient and see which antibiotic or combination works best, i.e., to personalize the treatment and not rely on what works in a general population. Every person has a slightly different response to treatment, even with the very same sickness. It's because of their bioflora, metabolic individuality and many other things. So the new device is a step toward more personalized medicine. But it can be very helpful not only for a particular patient, but also for scientific purposes like finding new, non-obvious combinations of antibiotics that work better than known ones."
Although the work was done on bacteria and their antibiotic susceptibility, the method has the potential to be upgraded and after further testing used, for example, for printing primers and doing digital PCR to identify specific genes or antibodies—especially with a single chip would cost no more than €5.
Microfluidic methods also have an extra advantage—when searching for new drugs, scientists often have a very limited amount of a potentially useful substance. Thanks to non-contact printing, they can test different concentrations and combinations of a potential cure without running out of the substrate too early.
More information: Adam S. Opalski et al, Combinatorial Antimicrobial Susceptibility Testing Enabled by Non-Contact Printing, Micromachines (2020). DOI: 10.3390/mi11020142
Provided by Polish Academy of Sciences