Nanocontainers for targeted drug delivery
RUDN University bioengineers have created magnetic nanocontainers for smart delivery of drugs to the desired organs or tissues, which reduces the risk of side effects. An experiment on mice determined that the nanocontainers are non-toxic. The results of the study are published in the journal Polymers.
Pharmaceutical side effects often occur because the active substance of the drug enters healthy organs. That is why, for example, chemotherapy is so hard for patients in the treatment of cancer: Toxic drugs affect not only tumor cells, but the whole body. Targeted drug delivery systems solve this problem. Many potential carriers have been proposed in recent years: microcapsules with a shell of polyelectrolytes, artificial liposomes of micro- and nanoscale, and protein nanoparticles, for example. Several dozen drugs packed in such containers are already used in practice or are undergoing clinical trials.
However, there are still many problems that prevent the widespread use of smart carriers. One is that the dependence of the drug biodistribution process in tissues dictates the size of containers. The smaller the size, the greater the likelihood that the drug will reach the correct organ, and the lower the dose of the drug is required, reducing toxic effects. Another problem is the lack of information about toxicity, effects on the body and distribution in living tissues. Both of these problems have been successfully solved by the RUDN University biochemists in collaboration with colleagues from Russia and the UK.
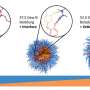
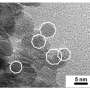
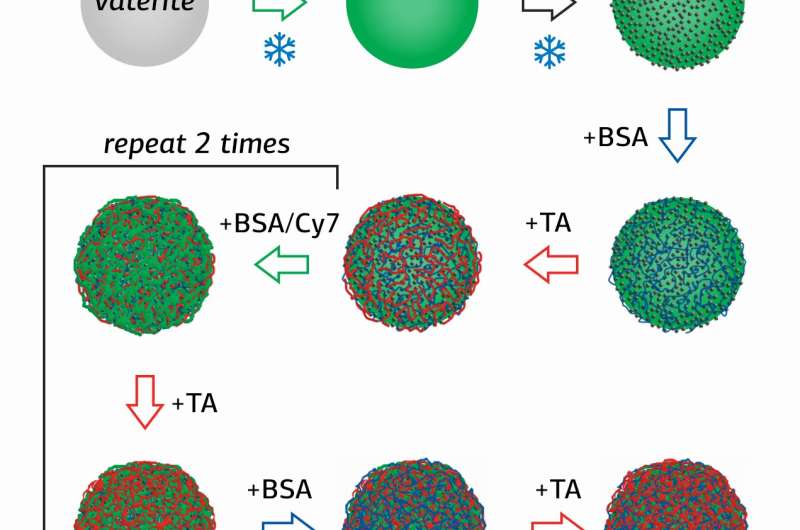
Researcher of the Surface Engineering Laboratory of RUDN University Olga Sindeeva and her co-authors created submicron-scale magnetic-sensitive containers –particles of 400-600 nanometers, with a shell of several layers of bovine serum albumin (BSA) with a fluorescent tag Cy7, and tannic acid (TA).
The novelty of the study is in the method of obtaining containers, in which nanoparticles of magnetite (MNPs), mixed iron oxide (II, III) were first adsorbed on the surface of porous granules of calcium carbonate, which were then coated sequentially with several layers of BSA-Cy7 and TA. Then, сalcium carbonate was washed out of the containers using an aqueous solution with a chelating agent.
"With this method, it was possible to double the amount of magnetite in containers compared to what is obtained by adsorption and co-deposition methods. Thus, it is possible to increase the magnetic moment of nanocontainers and increase the speed of their movement in the vascular system," Olga Sindeeva explained.
RUDN University bioengineers expect the submicron size of the containers to increase the bioavailability of the drug that is loaded into the MNPs (BSA-Cy7-TA) container.
Preliminary experiments on two cell lines, HeLa and fibroblasts, have shown that the containers do not affect cell viability and can be used in vivo.
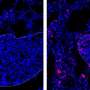
The drug-free containers were then tested on live BALB/c mice of both sexes weighing about 20 grams, 10 individuals per group. Containers in the form of a suspension in saline solution were injected into the tail vein of anesthetized mice. A suspension of magnetite-free containers (BSA-Cy7-TA) was used as a control. Then, one of the hind legs of the mice was exposed to a magnetic field for an hour while the other was left free for comparison. The distribution of nanocontainers in the tissues of living mice was observed using magnetic resonance imaging (MRI) and fluorescent tomography. Magnetometric analysis and histological examination of postmortem mice tissues were also performed one hour after removal of the magnet.
RUDN University biologists have shown that in the peripheral vessels of the hind limbs at rest at a low blood flow rate, MNPs(BSA-Cy7-TA) particles move in the first hour after intravenous injection in the direction of the limb to which the magnet is attached.
MRI showed that the concentration of magnetite in the muscle near the magnet passes through the maximum. The magnetite amount was found to be 70 percent higher than in the free limb. Then, the magnetite signal dropped to background values.
According to the results of histological studies and magnetometry, the researchers found that MNPs (BSA-Cy7-TA) concentrated mainly in the lungs, and, to a lesser degree, in the liver and spleen. Moreover, their concentration in the lungs was four to five times higher. A small amount of the carrier was also found in other internal organs and muscles, but concentration was significantly lower than in the lungs. Thus, biochemists concluded that the distribution of intravenous containers depends on the blood supply to the organs, that is, on the speed of blood flow, but is sensitive to the localization of the magnetic field.
Particular attention was paid to the toxicity of intravenous containers and their effects on the body. Preliminary tests have shown that in vitro in plasma or blood, a significant percentage of the containers is destroyed over the course of a day. The results of the studies suggest that the containers have time to achieve the goal with intravenous injection. Then, by changing the fluorescence signal, the carrier particles gradually degrade and are excreted from the body.
The particles are non-toxic and hemocompatible, and their size allows them to penetrate tissues of the body, but in working doses, they do not harm the respiratory or circulatory system, and do not affect kidney or liver functions. The activation of the complement system that is necessary for the biodegradation of the protein membrane of the containers does not affect the level of leukocytes, and therefore does not lead to any noticeable systematic inflammation.
Thus, the RUDN University researchers were able to engineer and distribute containers with a high amount of magnetite in the body, and effectively manage their deployment using a magnetic field.
In the future, the project participants intend to create smart nanocapsules that can deliver the drug to the correct organ and open to release the active substance. This method of drug delivery would avoid the side effects of treatment. Patients with a range of diseases, including children or elderly people with poor health, could be treated using drugs that might otherwise be avoided due to side effects that worsen the patient's condition.
More information: Marina V. Novoselova et al. Submicron-Sized Nanocomposite Magnetic-Sensitive Carriers: Controllable Organ Distribution and Biological Effects, Polymers (2019). DOI: 10.3390/polym11061082
Provided by RUDN University