Chemists close gap in making nanomedicines safer, more efficient

Dr. Jie Zheng believes he's turned a barrier into a bridge when it comes to nanomedicine implementation.
The professor of chemistry and his research team at The University of Texas at Dallas have demonstrated that nanomedicines can be designed to interface with a natural detoxification process in the liver to improve their disease targeting while minimizing potential side effects.
Their study, published July 15 in Nature Nanotechnology, indicates a path to making nanomedicine safer and more efficient.
"People have been working on nanomedicine for decades. It has great potential to advance cancer treatment and detection," said Zheng, the Cecil H. and Ida Green Professor in Systems Biology Science in the Department of Chemistry and Biochemistry at UT Dallas. "But there are potential hazards as well."
Nanomedicine broadly refers to the use of engineered nanoparticles, defined by their microscopic dimensions, for various health-related purposes. Primary among those roles are the pinpoint delivery of drugs and the detection of various diseases.
The liver, the largest detoxification organ in the body, captures and removes many substances originating both inside and outside the body.
"The liver protects us every day from damage from foreign materials," Zheng said. "But it is also a long-standing barrier to making safe and effective nanomedicines that patients can use."
Although many nanomedicines target disease efficiently in preclinical studies, Zheng said few of them reach clinical use. This is because, in the liver, macrophages—a type of white blood cell—capture and store them in the body long term, reducing their effectiveness and increasing their toxicity.
"The challenge is maximizing their treatment potential while minimizing side effects," he said. "Only when you solve both problems can you really bring this to the clinic."
The researchers' key discovery, conducted in a mouse model, is that one of the liver's natural toxin-removal processes can be used to enhance the delivery of nanomedicines while also making them safe. This process—glutathione-mediated biotransformation—eliminates the off-target nanomedicines so that they don't proceed to harm the body.
"We use this liver biotransformation as a way to modify the circulating nanomedicines so that macrophage uptake will be reduced," said Dr. Xingya Jiang, the lead author of the study. "With this liver biotransformation, the nanomedicines that miss the target can effectively clear out without long-term accumulation in the body."
This biotransformation was previously known to eliminate fatty molecules and small toxins, such as heavy metals. But its interaction with nanomedicines was unclear before this study.
"Liver cells constantly excrete glutathione to the sinusoid, which is the capillary in the liver. This glutathione excretion, called efflux, can transform the surface chemistry of nanoparticles so that the body can more easily eliminate them," Zheng said.
"Coupled with other physiological processes, this efflux can precisely control the transport of nanomedicines in the body, improving their targeting to the tumor and reducing their nonspecific accumulation in healthy tissues in the meantime," he said.
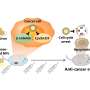
Along with Dr. Bujie Du, Zheng and Jiang designed a nanoprobe that uses organic dye to report how the biotransformation alters the nanoparticle and to better understand both its targeting and clearance.
Once the nanoprobe was delivered into the liver, the fluorescence of the dye was rapidly activated, indicating that the dye was dissociated from the nanoparticle in the liver.
"It wasn't certain before what happened when the nanoprobe came into the liver," Jiang said. "We hypothesized that there was some interaction in the liver that caused the dissociation, but we didn't really know. Now we've seen how it works."
The team validated what occurs in the liver by using nanoparticles of a precise size and well-defined structure; in this case, the particles each contained 25 gold atoms and four dye molecules. Knowing exactly how these nanoparticles were structured when they entered the body allowed accurate interpretation of how they differed when they cleared out of the body.
"As we monitored it, we saw that tumor targeting of nanomedicines significantly increased compared to controls, while the residual nanomedicines in normal tissues were minimized," Zheng said. "Because of this atomically precise design, we were also able to discover that the amino acid cysteine is also involved in this biotransformation process, helping modify these nanoparticles in vivo."
Zheng emphasized that this research demonstrates a new pathway for designing nanomedicines by taking advantage of the body's natural responses.
"Most people think of liver uptake as a barrier to nanomedicine delivery—that the liver is going to take them up and keep them in the body for a long time. This is a new strategy," he said. "We've made the liver behavior that we once considered a disadvantage to clinical translation of nanomedicines into an advantage.
"More than just providing a new strategy, we hope this inspires us to be creative thinkers so that many barriers in our research could become bridges to bigger scientific discoveries."
More information: Xingya Jiang et al. Glutathione-mediated biotransformation in the liver modulates nanoparticle transport, Nature Nanotechnology (2019). DOI: 10.1038/s41565-019-0499-6
Journal information: Nature Nanotechnology
Provided by University of Texas at Dallas