Lasers aim to replace scalpels in cutting-edge biopsy technique
To a patient, the analysis of a tissue biopsy sample to check for something like cancer may seem like a relatively simple process, even if it does mean giving up a small piece of flesh to be tested. The sample heads off to a lab, the patient heads home, and in several days the doctor calls with the results.
In reality, quite a bit of work goes into preparing a tissue sample and evaluating it for signs of disease. To be viewed under a microscope, the sample needs to be cut into extremely thin slices that might be only a few cells thick. And to aid with viewing, the technician may employ a variety of dyes to label specific proteins or cell structures.
"Extensive processing of the sample is required," says Lihong Wang, Caltech's Bren Professor of Medical Engineering and Electrical Engineering in the Division of Engineering and Applied Science. "You can only label so many molecules at a time, and you have to do a washing between labelings. And some molecules don't absorb dyes and don't get labeled at all."
A new technique being developed in Wang's lab aims to make that process a lot simpler and less invasive. Instead of using dyes, the technique uses pulses of laser light to image a sample.
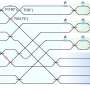
This new approach, called ultraviolet-localized mid-infrared photoacoustic microscopy, or ULM-PAM, develops images of the microscopic structures found in a piece of tissue by bombarding the sample with both infrared and ultraviolet laser light.
A sample to be imaged is first hit with a pulse of ultraviolet laser light. This light causes the molecules inside the sample to vibrate. Sensors placed against the sample pick up those vibration signals and pass them along to a computer that processes them.
In the next step, the sample is hit with a pulse of infrared laser light. This pulse heats the sample slightly but not evenly. Some materials in the sample, like proteins or DNA, will heat up more than others because they absorb more energy from the laser.
Immediately after the heating pulse, the sample is again hit with a pulse of ultraviolet laser light. Just as before, the UV light causes molecules inside the sample to vibrate, and those signals are passed along to the computer. By comparing the signals from samples before and after they are heated, the computer creates an image in which structures can be identified by their heat signatures. Since cancerous cells express proteins and DNA differently than healthy cells, they can be differentiated this way.
To better understand how it works, imagine if you were given two sheets of paper—one white and one black—and asked to determine which was which without looking at them.
One way to do that would be to set both sheets of paper in the sun, wait a few minutes, and then take their temperature. Because black objects absorb more light than white objects, the black sheet would get hotter than the white one. The sunlight in this example is analogous to the infrared laser used in the ULM-PAM technique, and the thermometer is analogous to the UV laser.
Junhui Shi, a postdoctoral scholar in medical engineering in Wang's lab, led the two-year effort to develop ULM-PAM and says the project faced some significant hurdles.
"Because ultraviolet light and infrared have different properties, we had to find special mirrors and glass that could focus both," he says. "And because no camera exists that can see both, we had to develop ways to see if they were correctly focused."
Though Wang and Shi have shown that ULM-PAM works, their technique remains at the proof-of-concept stage. It still takes too long to be useful in a clinical setting—although upgrading the lasers will allow quicker scans of tissue samples, they say.
A longer-term goal is to develop the technology into something that can be used on tissues while they are still in a patient's body, Wang says.
"I want to move this to in vivo. I want to use this to image cancer cells during surgery," he says. "That would be the dream."
The paper describing the technique, titled "High-resolution, high-contrast mid-infrared imaging of fresh biological samples with ultraviolet-localized photoacoustic microscopy," appears in the May 13 issue of Nature Photonics.
More information: Junhui Shi et al. High-resolution, high-contrast mid-infrared imaging of fresh biological samples with ultraviolet-localized photoacoustic microscopy, Nature Photonics (2019). DOI: 10.1038/s41566-019-0441-3
Journal information: Nature Photonics
Provided by California Institute of Technology