More realistic and accurate organs-on-chips

In a step toward better diagnosis and treatment of digestive conditions, such as inflammatory bowel disease, scientists report in ACS Biomaterials & Engineering that they have developed a first-of-its-kind collagen-based membrane for use in microchips. The membrane is more natural than others that are available, and it could allow organs-on-chips to more accurately replicate how healthy intestinal cells become diseased and how they react to drug treatments.
Traditionally, scientists have cultured cells on laboratory dishes and have used animal models to study disease and its potential treatments. But neither of these approaches fully mimic what occurs in the human body. Recently, researchers developed a way to grow living cells in microfluidic chips. Commonly called an organ-on-a-chip, each device is typically composed of a pair of flexible, translucent polymers or plastics that surround a porous membrane. Human cells extracted from an organ can be grown on the polymer or on the membrane. However, because the membrane itself is often made of plastic, it can disrupt cell interactions and skew the results. So, Abhinav Bhushan and colleagues at Illinois Institute of Technology sought to create a more natural membrane that would encourage the normal growth and development of human cells.
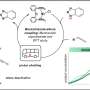
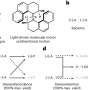
The researchers produced three types of microfluidic devices. One had no membrane, and the second had a plastic-derived membrane. For the third device, the research team used collagen to form the membrane. Collagen is one of the most common proteins in the body, and it helps form connective tissues. Then, they placed human colon cells in each device. After 5 days, microscopic evaluation revealed that colon cells on the collagen membrane were far more viable compared to those grown in the other devices. In addition, the cells grown on the collagen membrane were more differentiated. They also appeared to be integrating with the collagen fibers to remodel the microenvironment. The researchers concluded that using collagen-based membranes in organ-on-a-chip devices enhance the growth, viability and barrier function of human colon cells and that the method likely could be extended to cells from other organs.
More information: Chengyao Wang et al. Novel Microfluidic Colon with an Extracellular Matrix Membrane, ACS Biomaterials Science & Engineering (2018). DOI: 10.1021/acsbiomaterials.7b00883
Abstract
Collagen is a key element of basal lamina in physiological systems that participates in cell and tissue culture. Its function is for cell maintenance and growth, angiogenesis, disease progression, and immunology. The goal of our present study was to integrate a micrometer resolution membrane that is synthesized out of rat-tail type I collagen in a microfluidic device with apical and basolateral chambers. The collagen membrane was generated by lyophilization. In order to evaluate the compatibility of the resulting membrane with organs-on-chips technology, it was sandwiched between layers of polydimethylsiloxane (PDMS) that had been prepared by replica molding, and the device was used to culture human colon caco 2 cells on the top of the membrane. Membrane microstructure, transport, and cell viability in the organs-on-chips were observed to confirm the suitability of our resulting membrane. Through transport studies, we compared diffusion of two different membranes: Transwell and our resulting collagen membrane. We found that mass transport of 40 kDa dextran was an order of magnitude higher through the collagen membrane than that through the Transwell membrane. Human colon caco 2 cells were cultured in devices with no, Transwell, or ECM membrane to evaluate the compatibility of cells on the ECM membrane compared to the other two membranes. We found that caco 2 cells cultured on the collagen membrane had excellent viability and function for extended periods of time compared to the other two devices. Our results indicate a substantial improvement in establishing a physiological microenvironment for in vitro organs-on-chips.
Provided by American Chemical Society