Predatory bacteria found in study of cystic fibrosis patients' lung microbiome
Cystic fibrosis patients have a wide variety of bacteria in their lungs, including two 'predators' not detected before, according to a new study of lung microorganisms published this week in mBio, an online open-access journal of the American Society for Microbiology.
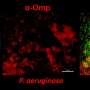
Using a laboratory technique called next-generation sequencing, a group of investigators from Madrid, Spain, studied the bacterial makeup of sputum samples provided by 15 cystic fibrosis patients three to four times over the course of a year. They found a wide range of bacterial species in the samples, including Pseudomonas aeruginosa, Staphylococcus aureus, Burkholderia and Pandorea. Each patient had his or her own bacterial makeup that remained relatively steady over the study period.
What surprised researchers was also finding two types of predator bacteria among the samples. Vampirovibrio, a bacteria that destroys cells by sucking out its contents, was found in 17 samples from 12 patients, while Bdellovibrio, which enters cells and feeds on its proteins, was found in six samples from three patients. The two types were found together in only one patient. Developing a novel computer science model to explain the relationship between these predators and potential prey bacteria, the investigators hypothesized that the predators, in the early stage of disease, may prevent the colonization of bacteria like P. aeruginosa normally associated with cystic fibrosis.
Predator bacteria "are ubiquitous and usually found in environmental aquatic ecosystems," said senior study author Rosa del Campo, of the Microbiology Service at Ramón y Cayal University Hospital. "In humans, a recent study has found them in the intestinal microbiota of healthy individuals and in patients with cystic fibrosis."
The findings indicate that "the lung microbiota in cystic fibrosis patients is more complex than we believed," she said. "Our study suggests that predatory bacteria could be used as a therapeutic strategy to reduce the bacterial load of the lungs of these patients."
Del Campo and colleagues analyzed 56 sputum samples from cystic fibrosis patients at her hospital. Patients were classified by lung function impairment as mild (five patients), moderate (nine patients), or severe (one patient). Among the samples, they found 156 types of bacteria, including Pseudomonas, Haemophilus, Staphylococcus, Pandoraea, Sphingomonas, Saccharibacteria genera incertae sedis, Stenotrophomonas, Leptotrichia, Capnocytophaga, Burkholderia, Oribacterium, Aquabacterium, Lachnoanaerobaculum, Campylobacter and Mycoplasma. P. aeruginosa and S. aureus were found together in the eight patients with the poorest lung function.
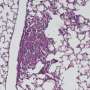
The natural evolution of cystic fibrosis is a progressive decline in lung function caused by a vicious circle of inflammation and tissue destruction, which is triggered and maintained by the chronic bacterial colonization of the lower respiratory tract, del Campo said. "It is generally acknowledged that once bacterial colonization is established in the lung, its eradication is almost impossible, despite consistent antibiotic treatment," she said.
The next steps for her team include cultivating the predator bacteria to understand their ability to survive in the lungs and their interaction with prey, and to try using predator bacteria to control the CF lung microbiota, she said.
Journal information: mBio
Provided by American Society for Microbiology