An end to cavities for people with sensitive teeth?
An ice cold drink is refreshing in the summer, but for people with sensitive teeth, it can cause a painful jolt in the mouth. This condition can be treated, but many current approaches don't last long. Now researchers report in the journal ACS Applied Materials & Interfaces the development of a new material with an extract from green tea that could fix this problem—and help prevent cavities in these susceptible patients.
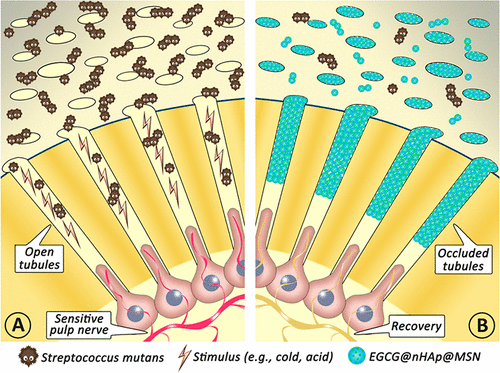
Tooth sensitivity commonly occurs when the protective layers of teeth are worn away, revealing a bony tissue called dentin. This tissue contains microscopic hollow tubes that, when exposed, allow hot and cold liquids and food to contact the underlying nerve endings in the teeth, causing pain. Unprotected dentin is also vulnerable to cavity formation. Plugging these tubes with a mineral called nanohydroxyapatite is a long-standing approach to treating sensitivity. But the material doesn't stand up well to regular brushing, grinding, erosion or acid produced by cavity-causing bacteria. Cui Huang and colleagues wanted to tackle sensitivity and beat the bacteria at the same time.
The researchers encapsulated nanohydroxyapatite and a green tea polyphenol—epigallocatechin-3-gallate, or EGCG—in silica nanoparticles, which can stand up to acid and wear and tear. EGCG has been shown in previous studies to fight Streptococcus mutans, which forms biofilms that cause cavities. Testing on extracted wisdom teeth showed that the material plugged the dentin tubules, released EGCG for at least 96 hours, stood up to tooth erosion and brushing and prevented biofilm formation. It also showed low toxicity. Based on these findings, the researchers say the material could indeed be a good candidate for combating tooth sensitivity and cavities.
More information: Jian Yu et al. Development of Epigallocatechin-3-gallate-Encapsulated Nanohydroxyapatite/Mesoporous Silica for Therapeutic Management of Dentin Surface, ACS Applied Materials & Interfaces (2017). DOI: 10.1021/acsami.7b06597
Abstract
In dental clinic, unsatisfactory management of the dentin surface after dentin exposure often leads to the occurrence of dentin hypersensitivity and caries. Current approaches can occlude the tubules on the dentin surface to relieve dentin hypersensitivity; however, the blocked tubules are generally weak in combating daily tooth erosion and abrasion. Moreover, cariogenic bacteria, such as Streptococcus mutans, produce biofilm on the dentin surface, causing caries and compromising the tubules' sealing efficacy. To overcome this problem, the present study focused on establishing a versatile biomaterial, epigallocatechin-3-gallate-encapsulated nanohydroxyapatite/mesoporous silica nanoparticle (EGCG@nHAp@MSN), for therapeutic management of the dentin surface. The effectiveness of the biomaterial on dentinal tubule occlusion, including resistances against acid and abrasion, was evaluated by field-emission scanning electron microscopy (FESEM) and dentin permeability measurement. The inhibitory capability of the biomaterial on S. mutans biofilm formation was investigated by confocal laser scanning microscopy (CLSM), 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay, colony forming units (CFU) counts, and FESEM. Results demonstrated for the first time that the use of EGCG@nHAp@MSN on the dentin surface was capable of effectively occluding dentinal tubules, reducing dentin permeability, and achieving favorable acid- and abrasion-resistant stability. Furthermore, EGCG@nHAp@MSN held the capability to continuously release EGCG, Ca, and P, and significantly inhibit the formation and growth of S. mutans biofilm on the dentin surface. Thus, the development of EGCG@nHAp@MSN bridges the gap between multifunctional concept and dental clinical practice and is promising in providing dentists a therapeutic strategy for the management of the dentin surface to counter dentin hypersensitivity and caries.
Journal information: ACS Applied Materials and Interfaces
Provided by American Chemical Society



















