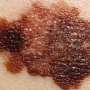
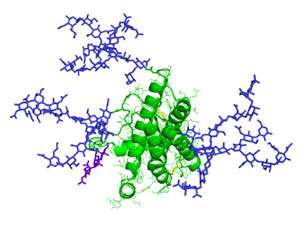
The body relies on thousands of sugar–protein complexes to stay healthy
Over two weeks in 2004, Song Zhiwei witnessed the slow death of a colony of cells. Song, a bioengineer at the A*STAR Bioprocessing Technology Institute (BTI), had bathed a plate of Chinese hamster ovary cells (CHO) with lectin, a toxic protein derived from plants. He then observed the millions of cells shrink to a dozen survivors. They looked average, but Song knew they had superpowers. The secret was hidden in the sweetening.
Sugars are essential for life. Among the most important class of sugars are those that are chemically attached to proteins. These glycoproteins are involved in everything from recognizing immune system invaders to lubricating membranes and stimulating the thyroid. They also fuel a booming pharmaceutical industry—many household drugs contain glycoproteins, and biotech companies invest significant resources in optimizing the sugaring of these proteins to improve their bioactivity and therapeutic potency.
Lectin is known to bind to sugars dangling on the ends of glycoproteins. In Song's experiment, only mutant CHO cells that did not produce those binding sugars could survive the lectin treatment. This approach of 'seeing what sticks' is an established method of identifying mutants that can subsequently be mass-produced by the biotech industry.
Song spent the next two years conducting cell culture experiments, molecular biology studies and genetic tests to prove that the cells were actually mutants. Determining the exact structure of the mutant glycoproteins required help from his colleague Lee May May, who headed the analytics group at BTI. May used mass spectrometry tools to determine the exact biochemical structure of the proteins produced by Song's mutant cells, revealing that they lacked key sugars. Song had created the first sugar-mutant cell lines applicable to biotech manufacturing.
The collaboration has since expanded into a globally renowned partnership between bioengineers and bioanalysts at A*STAR, advancing understanding of the role of sugars in disease.
Sweet talk
Sugars are the smallest and simplest form of carbohydrate, made of single or connected molecular units of carbon, hydrogen and oxygen. Our blood contains hundreds of types of sugars: some floating freely, but many more attached to proteins like decorations on a Christmas tree. Almost 70 per cent of the proteins in our body are glycosylated, which means that they won't function without their sugary accoutrement. The specific arrangement of sugars, or glycans, on a glycoprotein determines how a protein folds and interacts with other molecules, alters its solubility and sometimes even the messages it transmits to cells. "The cell expends an enormous amount of energy to put sugars on proteins," says Pauline Rudd, a veteran in the field of glycobiology, who joined the BTI analytics team in 2015. "If you didn't have sugars, you wouldn't survive."
Researchers first discovered the critical role of glycoproteins in the early 1900s. An Austrian physician, Karl Landsteiner, noticed that human blood mixed with the blood of animals, or even other humans, forms clumps. These clumps can clog vessels or crack open to release toxic proteins into the body. However, Landsteiner noticed that some blends did not coagulate. This discovery led him to the blood-group classification still used today—A, B, AB and O—and won him the Nobel Prize in Physiology or Medicine in 1930. In the 1950s researchers determined that the sugars exposed on the surface of red blood cells determined which blood group they belonged to.
The blood work encouraged research into glycoproteins. By the 1990s, biologists were caught up in the genetics craze. The cure for everything, they posited, was hidden in our DNA. "Genes were claimed to be the cause of everything," says Rudd, who saw funding for glycobiology wane. Between 1998 and 2000, $3.5 billion was spent globally on genomics research, including the initiative to sequence the entire human genome. "There was a lot of information but it didn't give us a direct route to understanding disease," says Rudd. "People began to suggest that maybe genes don't do anything except code for proteins."
Scientists shifted their attention to the many other stages of biological activity until they arrived again at sugars.
"DNA is the first layer of information. This information is transcribed into RNA, which sends a message that is translated into a protein with a function," says Song. "Carbohydrates, or sugars, are the last layer of biological information."
Knowing the importance of sugars didn't make them any easier to study. DNA and proteins are essentially linear structures that "curl up into fancy shapes," says Rudd. Sugars branch out into multiple chains. "They are like big trees hanging off the sides of proteins." It would take several years before sugars could be analyzed with the precision and speed of genes and proteins.
Shake up
In 1989 an earthquake hit California. Rudd remembers it well. She was deep into a collaboration between the Oxford Glycobiology Institute (led by Director Raymond Dwek) and a research team in London, looking for changes in the way proteins are glycosylated in patients with autoimmune diseases. She was analyzing 600 samples of the immunoglobulin G (IgG) protein, using a special gel to filter the sugars. The factory that produced this gel was destroyed by the earthquake.
When the factory was rebuilt, its gel was not the same. "It was completely useless," remembers Rudd. "I was tearing my hair out trying to get these 600 samples analyzed."
Necessity breeds invention, so Rudd looked around and noticed the liquid chromatography (LC) columns she had been using to sort proteins. She stuck a syringe filled with a mixture of sugars released from her glycoprotein samples into the columns. The LC device filtered the sugars to a much higher resolution than the gel process. "We never went back," she says.
Since then, Rudd has collaborated with private and institutional partners to speed up, automate and improve the specificity of techniques for sorting and characterizing sugars from a sample. What used to take a year can now be done in a day. The workflow, bioinformatics and databases developed by Rudd's team at the National Institute for Bioprocessing Research and Training (Dublin, Ireland) have been incorporated into Waters Corporation's UNIFI analytical coupled liquid chromatography/mass spectrometry platform, which means that much of the complexity of glycoanalysis is now automated. Hence, glycoanalysis has entered a new era of glycomics, bringing it closer to the big-data universe of genetics, transcriptomics and proteomics.
"We can now look at large cohorts of samples to understand more about diseases and to support biologic development and production," says Terry Nguyen-Khuong, who heads the analytics group at BTI. Since teaming up with Rudd, A*STAR has expanded its analytics portfolio to zoom in on sugars and identify their exact location, basic building blocks and linking structures.
Pharming glycoproteins
Glycoproteins fuel a US$163 billion biopharma industry of drugs whose efficacy can be dictated by sugars. For example, when the hormone erythropoietin is adorned with sialic acid sugars, it is ten times more effective at stimulating red blood cell production in anemic patients than the hormone alone.
In the glycoprotein business, CHO cells comprise the entire workforce. They can produce any proteins the biotech industry demands, and can sugar-coat the proteins in the same way humans do.
Before Song created his first CHO-cell mutants, no-one had been able to control the glycosylation of proteins in mass-producible cell lines. Pamela Stanley's group in the United States had been tweaking the glycosylation of CHO cells for years using cell lines that lived and died on a flat petri dish, fed on protein-rich cow's blood. Song instead developed mutants using cells that he knew could replicate indefinitely while swirling in spherical 20,000-liter bioreactors used in biopharma factories—free of bovine additives.
He named the cell line CHO-glycosylation mutant 1 (GMT-1), and since then, more than twenty successors have followed in numerical order. When tools emerged that made editing genes as simple as cutting and pasting words on a computer screen, he used them to generate more mutants.
In GMT-3, he deleted a gene required to fix fucose sugars to proteins. GMT-9 glycoproteins lack the sugars fucose and galactose; and GMT-17 lacks fucose, galactose and sialic acid. The absence of these sugars can dictate the potency of drugs. Song's cells produce antibodies that are up to a hundred times better at killing cancer cells than their equivalent drugs in the market, such as rituximab (branded Rituxan) to treat leukemia. "The cell lines are comparable to industrial lines and are ready for commercialization," says Song, who has been managing a S$11 million glycomics grant called GlycoSing since 2014. Treatments with these improved antibodies would mean significantly reduced doses.
In 2008, Andre Choo, a researcher at BTI, developed the first antibodies that could specifically kill embryonic stem cells, alleviating concerns about the cells forming tumors in transplant patients. The antibodies have since been licensed to several companies.
Many diseases have a distinct sugar profile, a concept that Choo has begun to exploit for cancer therapeutics. He screens for antibodies that specifically target aberrant sugar molecules on the surface of cancer cells, working with Rudd and Nguyen-Khuong's team to analyze them.
Recently this year, his team generated an antibody that recognizes sugars expressed on ovarian cancer cells. "In the past we would generate an antibody without really knowing what it targeted, we are now focused on trying to get these anti-glycan antibodies."
At A*STAR, research has expanded into dengue, the Zika virus and heart disease. "All major areas in medicine—cancer, infectious disease and inflammatory problems—are related to glycoproteins," says Song, whose mutants could potentially cure these diseases.