April 6, 2017 report
Nanoparticles pass through mucus membranes in lungs to deliver pulmonary drugs

(Phys.org)—A team of researchers from multiple institutions in the U.S. has developed a new way to treat lung disease—using nanoparticles to transport chemicals through the thick mucus membranes that can coat pulmonary airways. In their paper published in the journal Science Advances, the team describes how they used particles small enough to move through holes in the mesh that makes up mucus to deliver helpful drugs.
Lung problems impact the lives of millions of people. Such conditions include asthma, in which bronchi spasm, making it difficult to breathe; cystic fibrosis, in which over-production of mucus leads to blocking of bronchi; and COPD, in which obstructions form in bronchial passages. Fortunately, these types of ailments are all treatable to some degree, though they cannot be cured. For that reason, scientists continue to look for ways to improve current therapies.
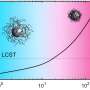
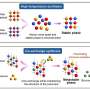
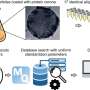
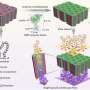
Currently, lung ailments such as cystic fibrosis, COPD and asthma are treated with inhaled drugs such as corticosteroids that adhere to the walls of air passages. In some instances, they are carried by what are known as mucoadhesive particles, (MAPs), but, as the researchers note, thick mucus often builds up on such passageways, lessening the effectiveness of the delivery system. In this new effort, the researchers took a different approach—rather than trying to make medicines that adhere do their job better, they turned to nanoparticles that are small enough to make their way through mucus membranes to the lining of the lungs themselves, offering direct medication application to affected areas. Called mucus-penetrating particles (MPP), they remain in the lungs, releasing medication for an extended period of time.
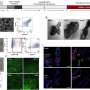
The nanoparticles, the team notes, were created using biodegradable materials that prior research found safe for internal use. Testing in mice, they report, showed the particle carriers stayed in the lungs for several hours—they also proved to be more effective than conventional therapies at reducing asthma symptoms such as irritation.
The researchers suggest that MPPs could offer a better treatment plan for lung patients by providing a therapy that maintains drug levels in the lungs for longer periods of time, reducing the need for repeated dosing, which itself can cause lung irritation.
More information: Craig S. Schneider et al. Nanoparticles that do not adhere to mucus provide uniform and long-lasting drug delivery to airways following inhalation, Science Advances (2017). DOI: 10.1126/sciadv.1601556
Abstract
Mucoadhesive particles (MAP) have been widely explored for pulmonary drug delivery because of their perceived benefits in improving particle residence in the lungs. However, retention of particles adhesively trapped in airway mucus may be limited by physiologic mucus clearance mechanisms. In contrast, particles that avoid mucoadhesion and have diameters smaller than mucus mesh spacings rapidly penetrate mucus layers [mucus-penetrating particles (MPP)], which we hypothesized would provide prolonged lung retention compared to MAP. We compared in vivo behaviors of variously sized, polystyrene-based MAP and MPP in the lungs following inhalation. MAP, regardless of particle size, were aggregated and poorly distributed throughout the airways, leading to rapid clearance from the lungs. Conversely, MPP as large as 300 nm exhibited uniform distribution and markedly enhanced retention compared to size-matched MAP. On the basis of these findings, we formulated biodegradable MPP (b-MPP) with an average diameter of <300 nm and examined their behavior following inhalation relative to similarly sized biodegradable MAP (b-MAP). Although b-MPP diffused rapidly through human airway mucus ex vivo, b-MAP did not. Rapid b-MPP movements in mucus ex vivo correlated to a more uniform distribution within the airways and enhanced lung retention time as compared to b-MAP. Furthermore, inhalation of b-MPP loaded with dexamethasone sodium phosphate (DP) significantly reduced inflammation in a mouse model of acute lung inflammation compared to both carrier-free DP and DP-loaded MAP. These studies provide a careful head-to-head comparison of MAP versus MPP following inhalation and challenge a long-standing dogma that favored the use of MAP for pulmonary drug delivery.
Journal information: Science Advances
© 2017 Phys.org