Research reveals new possibilities for islet and stem cell transplantation

(Edmonton) James Shapiro, one of the world's leading experts in emerging treatments of diabetes, can't help but be excited about his latest research. The results he says, could soon mark a new standard for treatment—not only in diabetes, but in several other diseases as well.
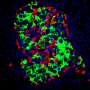
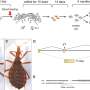
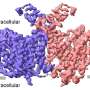
Shapiro, a Canada Research Chair in Transplantation Surgery and Regenerative Medicine in the University of Alberta's Faculty of Medicine & Dentistry, along with Andrew Pepper, a post-doctoral fellow working in his lab, are the lead authors in a study published in the April 20 edition of the journal Nature Biotechnology. In the study, the authors describe developing a new site for islet transplantation under the skin, which they believe will offer less risk and far greater health benefits for patients.
Islet transplantation is a procedure that temporarily allows severe diabetics to stop taking insulin.
"Until now it has been nearly impossible for transplanted cells to function reliably when placed beneath the skin," says Shapiro. "In these studies, we have harnessed the body's natural ability to respond to a foreign body by growing new enriching blood vessels. By controlling this reaction, we have successfully and reliably reversed diabetes in our preclinical models. This approach is new and especially exciting as it opens up a world of opportunities, not only in diabetes, but also across the board in regenerative medicine."
The new technique, tested in preclinical models, is an evolution of the Edmonton Protocol, which Shapiro developed in the late 1990s to treat Type 1 diabetes. In the Edmonton Protocol, islet cells are transplanted into the liver, granting patients insulin independence for a varying amount of time. While hailed as a revolutionary treatment at the time, Shapiro quickly realized the liver wasn't the ideal site for transplantation as most of the islets were destroyed in a matter of minutes to hours. As he considered the future possibility of transplanting human stem cells in place of islets, he realized a better, safer site to implant experimental cells was needed.
Shapiro's team began testing an alternative site underneath the skin, but at first it proved inhospitable for the cells due to a lack of blood vessels needed for the islets to grow and reproduce. As part of their research though, they found that by inserting a temporary catheter tube under the skin, new blood vessels could be induced to grow, making an ideal home for islet transplantation.
The researchers say the new procedure has the potential to be applied safety and easily to patients. They add, it not only offers several benefits to diabetes patients, but also could safely open the door to allow for the assessment of emerging stem cell treatments for other illnesses as well.
"It opens up the possibility of being able to transplant stem cells into patients in a site that can be removed," says Pepper. "That's been a big focus when you've got a new cell line that's never been tested in patients before. The ability to take the cells out if there's a problem is very important."
"This exciting new approach doesn't have to be limited to diabetes," says Shapiro. "For any area of regenerative medicine that requires replacing old cells with new - and there's lots of different disease states where there's just one gene defect that could be corrected by a cell transplant— this opens up an incredible future possibility for successful engraftment beneath the skin."
Shapiro has filed a patent for the new transplant technique and hopes to begin human trials in the very near future.
More information: A prevascularized subcutaneous device-less site for islet and cellular transplantation, Nature Biotechnology (2015) DOI: 10.1038/nbt.3211
Journal information: Nature Biotechnology