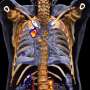
Prototype for first traceable PET-MR phantom

As cancer diagnostic tools, a new class of imagers – which combines positron-emission tomography (PET) with magnetic resonance imaging (MR or MRI) – has shown promise in the few years since these hybrid machines have been commercially available. But to thoroughly assess PET-MR scanners' clinical performance, researchers will need to calibrate the machines in a way that is traceable to a national standard.
Aiding that effort, a collaboration of NIST scientists from PML's Radioactivity and Magnetics groups has created a prototype of the world's first traceable phantom, or calibration standard, for a dedicated PET-MR imager.
PET-MR scanners may become an alternative in some cases to the commonly used PET-CT scanners, which combine PET's radioactive tracer-sensitive capabilities with the anatomical detail of x-ray computed tomography (CT). Though research is still needed to identify the best role for PET-MR, one advantage is minimizing patients' exposure to the ionizing radiation of a CT scan.
To build their prototype, the NIST team adapted a phantom that had been developed for MRI calibrations.
Nicknamed "Phannie," the original MRI phantom consists of a plastic sphere about the size of a person's head filled with grids of smaller plastic spheres containing salt solutions that become magnetized in a magnetic field. The new phantom prototype includes a small, calibrated amount of fluorine-18 (F-18), a radionuclide that shows up in PET images.
In initial studies carried out using NIST's PET-CT scanner, the researchers found that the PET imaging data were accurate to within 1.5%, which is good enough for most applications, though the team hopes eventually to increase this accuracy to less than 1%.
The next iteration of the prototype should be built and tested within a year and will feature a more robust and user-friendly design, including sturdier walls and an improved filling system that will make it easier and faster to introduce the radioactive solutions. The future model may also include calibrated samples of solid, longer-lived radioactive sources for tests that can further monitor PET scanner performance.
Provided by National Institute of Standards and Technology