Gelatin nanoparticles could deliver drugs to the brain

Stroke victims could have more time to seek treatment that could reduce harmful effects on the brain, thanks to tiny blobs of gelatin that could deliver the medication to the brain noninvasively.
University of Illinois researchers and colleagues in South Korea, led by U. of I. electrical and computer engineering senior research scientist Hyungsoo Choi and professor Kyekyoon "Kevin" Kim, published details about the gelatin nanoparticles in the journal Drug Delivery and Translational Research.
The researchers found that gelatin nanoparticles could be laced with medications for delivery to the brain, and that they could extend the treatment window for when a drug could be effective. Gelatin is biocompatible, biodegradable, and classified as "Generally Recognized as Safe" by the Food and Drug Administration. Once administered, the gelatin nanoparticles target damaged brain tissue thanks to an abundance of gelatin-munching enzymes produced in injured regions.
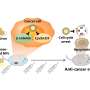
The tiny gelatin particles have a huge benefit: They can be administered nasally, a noninvasive and direct route to the brain. This allows the drug to bypass the blood-brain barrier, a biological fence that prevents the vast majority of drugs from entering the brain through the bloodstream.
"Overcoming the difficulty of delivering therapeutic agents to specific regions of the brain presents a major challenge to treatment of most neurological disorders," said Choi. "However, if drug substances can be transferred along the olfactory nerve cells, they can bypass the blood-brain barrier and enter the brain directly."
To test gelatin nanoparticles as a drug-delivery system, the researchers used the drug osteopontin (OPN), which in rats can help to reduce inflammation and prevent brain cell death if administered immediately after a stroke.
"It is crucial to treat ischemic strokes within three hours to improve the chances of recovery. However, a significant number of stroke victims don't get to the hospital in time for the treatment," Kim said.
By lacing gelatin nanoparticles with OPN, the researchers found that they could extend the treatment window in rats, so much so that treating a rat with nanoparticles six hours after a stroke showed the same efficacy rate as giving them OPN alone after one hour – 70 percent recovery of dead volume in the brain.
The researchers hope the gelatin nanoparticles, administered through the nasal cavity, can help deliver other drugs to more effectively treat a variety of brain injuries and neurological diseases.
"Gelatin nanoparticles are a delivery vehicle that could be used to deliver many therapeutics to the brain," Choi said. "They will be most effective in delivering drugs that cannot cross the blood-brain barrier. In addition, they can be used for drugs of high toxicity or a short half-life."
More information: "Gelatin nanoparticles enhance the neuroprotective effects of intranasally administered osteopontin in rat ischemic stroke model." Drug Delivery and Translational Research December 2014, Volume 4, Issue 5-6, pp 395-399 link.springer.com/article/10.1007%2Fs13346-014-0208-9
Journal information: Drug Delivery and Translational Research
Provided by University of Illinois at Urbana-Champaign