Scientists 'reprogram' mouse fat cells into clinically useful stem cells
Australian scientists from the Monash Institute of Medical Research have "reprogrammed" adult mouse fat cells and neural cells to become stem cells that can differentiate into a variety of different cells (pluripotency). The cells, called "induced pluripotent stem cells" (iPS), are nearly identical to the naturally occurring pluripotent stems cells, such as embryonic stem cells, which are highly pluripotent, in short supply and their access restricted in the U.S.
The study is published in issue 19(5) of Cell Transplantation and is now freely available on-line.
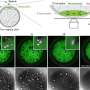
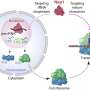
"Induced pluripotent stem cells have revolutionized cell reprogramming," said the study's lead author, Dr. Paul J. Verma. "One challenge is to find the most appropriate cell for reprogramming. Our study demonstrated that both neural stem cells (NSCs) and adipose tissue-derived cells (ADCs) from adult mice expressed genetic pluripotency and could differentiate into the three germ layers, endoderm, mesoderm and ectoderm. The ADCs were the most amenable to reprogramming."
According to Dr. Verma, iPS cells have been shown to have many of the hallmarks of embryonic stem cells. Choosing which cells were best for reprogramming required looking at the ease of access and ease of derivation and growth of the cells in vitro. They concluded that it was likely that certain iPS cell lines will have a "higher propensity to differentiate into certain lineages (cell types)."
"This variation may be related to different levels of programming achieved," added Dr. Verma. "Many different cell types need to be investigated to generate many iPS lines for specific differentiation and different research purposes."
The research team concluded that ADCs represent a more clinically relevant cell type and that fat tissue can be easily accessed and grown easily and rapidly in cultures. Fat tissue cells, when reprogrammed, can also be prolific. The authors cited a study previously published in Cell Transplantation (16:9) suggesting that 100 ml of human fat tissue could yield one million clinically useful stem cells.
Their work takes the development of iPS cells a step closer toward their eventual clinical use in treating human diseases.
"There is considerable potential in the generation of iPS cells for the treatment of a number of disorders" said Dr. Paul Sanberg, coeditor-in-chief and Director of the Center Of Excellence for Aging and Brain Repair at the University of South Florida. "Finding the optimal source of cells to start with, is of paramount importance and this study provides reassuring data on a highly favorable source".
Provided by Cell Transplantation Center of Excellence for Aging and Brain Repair