Hepatitis B patients' understanding of infection and treatment deficient
Many patients with chronic hepatitis B are deficient in their understanding of the lifelong disease and often do not comply with the drug regimens necessary to control it, according to a new UCLA survey that suggests improved patient involvement in disease management decisions could be the key to fixing this problem.
The national survey — funded by Idenix Pharmaceuticals and Novartis Pharma AG and presented May 20 during the annual Digestive Diseases Week conference in Washington, D.C. — indicates that patient involvement in disease management decisions need to be improved, which could result in better adherence to drug regimens and improved clinical outcomes.
“The results of this study are very compelling and are a wake-up call to physicians caring for hepatitis B patients that we need to educate our patients more about risk factors, modes of transmission and expectations regarding antiviral therapy,” said Dr. Steven-Huy Han, associate clinical professor of medicine and surgery in the division of digestive diseases at the David Geffen School of Medicine at UCLA and a consultant for both Idenix and Novartis.
The study was based on responses from 301 adult chronic hepatitis B patients on antiviral therapy. Of those, 24 percent were on interferon treatment. Most of these patients were males between the ages of 31 and 50, with about half being of Asian descent. In addition, 64 percent were from the mid-Atlantic or Pacific regions of the United States. The study was based on Internet interviews, supplemented by telephone interviews, conducted between September and November 2006.
Among the findings:
-- 36 percent of respondents mistakenly thought the virus could be spread through sharing utensils.
-- 80 percent were aware of the long-term consequences of the hepatitis B virus.
-- Half of the respondents erroneously believed a cure existed for the chronic virus, though just more than 60 percent had been in treatment for about a year.
-- 31 percent said they knew specific names of hepatitis B virus tests, but only half knew what the tests measured.
-- 85 percent felt that measuring virus levels was important, though 27 percent didn’t know if their physicians took those measurements.
-- 37 percent did not discuss treatment goals with their physicians, yet 88 percent of these respondents felt they should be doing this.
-- 51 percent felt involved in treatment decisions.
-- 54 percent were unsure why the drugs they were taking had been chosen.
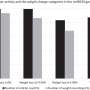
Respondents also admitted frequently missing doses or taking them at the wrong time. For instance, 12 percent admitted not complying once per month; 7 percent once every two weeks; 7 percent once a week; 7 percent two to three times per week; 1 percent four to six times per week; and 4 percent once per day. Also, 9 percent thought that missing one or two doses didn’t matter.
Source: University of California - Los Angeles