Scientists Discover Key to Growing New Stem Cells
Scientists at Duke University Medical Center have demonstrated they can grow human stem cells in the laboratory by blocking an enzyme that naturally triggers stem cells to mature and differentiate into specialized cells.
The discovery may enable scientists to rapidly grow stem cells and transplant them into patients with blood disorders, immune defects and select genetic diseases, said the Duke researchers.
Stem cells are the most flexible cells in the body, continually dividing into new stem cells or into specialized cells that carry out specific roles in the body. But little is known about how stem cells choose their fate. The Duke team focused on "hematopoietic" or blood stem cells.
In their study, the investigators discovered that an enzyme, aldehyde dehydrogenase (ALDH), stimulates hematopoietic stem cells to mature and transform into blood or immune cells, a process called differentiation. They inhibited this enzyme in stem cell cultures and successfully increased the number of stem cells by 3.4 fold. Moreover, they demonstrated the new stem cells were capable of fully rebuilding the blood-forming and immune systems of immune-deficient mice.
Results of the study are published on line and will be published in the August 10, 2006, issue of the Proceedings of the National Academy of Sciences.
"Our ability to treat human diseases is limited by our knowledge of how human stem cells determine their fate -- that is, whether they maintain their ability to self-renew or whether they go on to become specialized cells," said John Chute, M.D., associate professor of medicine in the Duke Adult Bone Marrow and Stem Cell Transplant Program. "Unraveling the pathways that regulate self-renewal or differentiation in human stem cells can facilitate our ability to expand the growth of human stem cells for therapeutic uses."
Currently, patients who require stem cell transplants are given either bone marrow from adult donors, umbilical cord blood derived from newborn babies, or stem cells from blood. But stem cells are scarce, representing less than 0.01 percent of the bone marrow cell population. Likewise, cord blood units frequently lack sufficient numbers of stem cells to rebuild a patient's decimated immune system.
Efforts to grow human hematopoietic stem cells in the laboratory have proven extraordinarily difficult, Chute said, because growth factors in culture make stem cells rapidly differentiate. The scientists searched for ways to block a stem cell's natural propensity to differentiate without promoting uncontrolled growth.
The researchers focused on the ALDH enzyme because it is a telltale "marker" that distinguishes stem cells from other blood and immune cells. Moreover, it is known to play an essential role in the body's production of retinoic acids, which regulate cell differentiation in a variety of tissues. Yet how ALDH functions in stem cells remained unknown, Chute said.
The scientists began by analyzing how stem cells behave under normal circumstances when grown in culture. They mixed together purified human stem cells with growth factors that induce stem cells to mature and differentiate. As expected, the stem cells showed a marked decline in number as they differentiated into other types of specialized cells. By day seven, all stem cells had disappeared from culture.
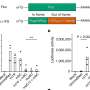
The scientists then added an inhibitor of ALDH to the stem cell cultures, and they found that half of the stem cells maintained their immature and undifferentiated status. Moreover, adding the inhibitor caused a 3.4-fold increase in stem cell numbers within seven days.
Next, the scientists transplanted the cultured stem cells into immune-deficient mice to determine how the stem cells would behave. The new population of stem cells migrated to the bone marrow as expected and successfully "engrafted," or took hold in the bone marrow, where they began to produce new blood and immune cells.
"ALDH appears to play a fundamental role in the differentiation program of human hematopoietic stem cells," Chute said. "Inhibition of this enzyme facilitates the expansion of human hematopoietic stem cells in culture."
Chute said their results reveal a unique role for both ALDH and the process of retinoic acid signaling in human stem cells. Chute and colleague Donald McDonnell, Ph.D., professor of pharmacology and cancer biology, are currently testing whether they can directly block the retinoic acid receptors in stem cells and produce a comparable expansion of human stem cells.
The investigators plan to develop a clinical trial to test their approach to expand human stem cells for therapeutic purposes.
Source: Duke University Medical Center