Designing touch-sensitive virtual reality tools to train and test tomorrow's surgeons
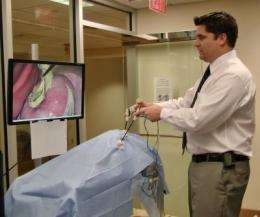
Minimally invasive surgery is increasingly common and effective for operating inside the human abdomen. In these laparoscopic procedures, which use slender, handheld tools inserted into the body of the patient, the skill of the surgeon is the most important factor determining the success of the operation. A team of interdisciplinary researchers led by Rensselaer Polytechnic Institute has won a $2.3 million federal grant to develop a touch-sensitive virtual reality simulator that will standardize how surgeons are trained and certified to perform laparoscopic procedures.
As surgeons perform most of the procedure with remote control tools that can be inserted into the body using only small incisions, laparoscopic surgery foregoes the need for large incisions and, in turn, usually results in shorter recovery times for patients. The skills needed to perform most minimally invasive laparoscopic operations - including, for example, gallbladder removal and gastric band surgery - can be reduced to a handful of basic tasks: cutting in very specific patterns, tying knots, stitching, and manipulating very small items. Studies show that being proficient at these tasks is critical for performing laparoscopic surgery.
The new four-year grant, awarded by the National Institute of Biomedical Imaging and Bioengineering at the National Institutes of Health, tasks Rensselaer Professor Suvranu De and his team of researchers with developing new hardware and software that effectively trains surgeons to perform these fundamental tasks, as well as objectively assesses the performance of physicians who are seeking to become certified in laparoscopic surgery. This new testing and training system will employ haptic technology, or touch feedback, which realistically replicates the sensation a surgeon would feel in his or her hands during an actual procedure. De, an expert in multiscale computer modeling and haptics, is joined by researchers at Beth Israel Deaconess Medical Center and Tufts University.
"We want to give surgeons the best tools possible, so they can better hone their skills and successfully treat their patients," said project leader De, associate professor in the Department of Mechanical, Aerospace, and Nuclear Engineering at Rensselaer. "Just as training on virtual reality simulators has shown to be highly effective for jet pilots, we know that physicians show increased success in surgery the more times they perform it. We're creating new tools that make it easier than ever for them to practice. These same tools will also be used in certification tests to make sure surgeons have all the required skills mastered before they start operating on patients."
It has been reported that physicians who performed less than 100 laparoscopic procedures have significantly more complication rates in contrast to experienced surgeons, De said. The new virtual reality simulator will be developed to adhere to the standard and recommendations laid out in the Fundamentals of Laparoscopic Surgery - a comprehensive program being developed by a joint committee of the Society of American Gastrointestinal Endoscopic Surgery (SAGES) and the American College of Surgeons (ACS) for training and credentialing surgeons.
The new system features real laparoscopic tools, which are connected to equipment nearly identical to that used in actual surgical situations. Realistic computer-generated models of the simulation scene are displayed on a monitor, and the users interact with simulation both visually and using their sense of touch. The haptics technology ensures that a physician cutting or stitching tissue with the simulator will feel with their hands the lifelike toughness, sponginess, and resistance of virtual tissue. By pairing haptics with automation, the simulator will also be able to literally guide the hands of trainees, so they can see and feel the correct movements as they learn specific surgical tasks. The research team plans to make these simulations available over the Internet.
To watch a video demo of a similar simulator:
De said the team expects the new system to significantly change the current paradigm of surgical education and assessment, in which performance is subjectively measured by exam administrators. The current system not only places a time burden on the individual being tested and the administrator, it generally requires travel as there are only a few test sites around the country. The new virtual reality simulator will assess test-takers objectively against board-certified standards and criteria, possibly over the Internet. The new system is also expected to be more cost effective, with a lower price point that should lead to a wider availability across the country.
After developing the new system, the research team will work to test and validate the effectiveness and usefulness of the system as a testing and training tool at the Carl J. Shapiro Simulation and Skills Center at Beth Israel Deaconess Medical Center in Boston.
Along with De, investigators working on this new study are Harvard Medical School Professor Daniel B. Jones and human factors engineering expert Caroline G. L. Cao, associate professor of mechanical engineering at Tufts University.
Provided by Rensselaer Polytechnic Institute