Diagnosing heart attacks may be a lick and a click away
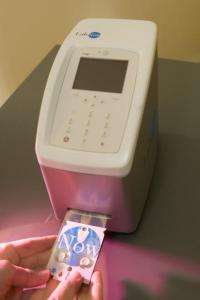
A diagnostic tool developed by Rice University scientists to detect heart attacks using a person's saliva is being tested at the Michael E. DeBakey VA Medical Center (MEDVAMC) in collaboration with Baylor College of Medicine (BCM) in Houston.
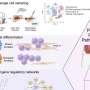
John T. McDevitt, professor of chemistry and bioengineering at Rice, and his team of researchers at Rice's BioScience Research Collaborative have developed a microchip sensor, the Nano-Bio-Chip, which processes saliva and yields on-the-spot results. McDevitt intends to establish Houston as the hub of a biomarker highway where Nano-Bio-Chips will be configured to diagnose a variety of diseases.
"The device works by analyzing saliva, looking for cardiac biomarkers of injury implicated in the heart attack," said Dr. Biykem Bozkurt, professor of medicine at BCM.
"We find salivary tests, when combined with electrocardiograms (ECG), can provide more accurate information than the ECG alone for patients with chest pain," McDevitt said. "Saliva-based tests have the potential to quickly diagnose heart-attack victims as well as to find false alarms."
Typically, when a heart attack occurs, emergency medical technicians or hospital staff use an ECG machine to review heart activity. If the ECG is abnormal, the patient is immediately moved to an area to be treated. Unfortunately, ECGs fail to correctly diagnose about a third of patients having a heart attack. These patients are monitored carefully in the emergency room, where further blood tests are used to look for certain biomarkers to verify whether a heart attack has occurred.
"At the DeBakey VA, we follow this same procedure but also include the saliva test to determine whether salivary biomarkers will perform similar to blood markers in diagnosing a heart attack," said Bozkurt, who is also chief of cardiology at the MEDVAMC. "The patients presenting with chest pain are enrolled from the VA emergency room after informed consent and provide a saliva swab as well as blood samples. It is anticipated that saliva will be an alternative or complementary technique to blood drawing for early diagnosis of heart attacks, ultimately for testing in the ambulance before arrival in the emergency room."
Over the next two years, samples from approximately 500 patients who come to the MEDVAMC emergency room with chest pain or heart attack-related symptoms will be collected.
To obtain a saliva sample for the Nano-Bio-Chip, health care providers swab a patient's gums with a cotton-tipped stick. The saliva is transferred to the disposable diagnostic microchip. The microchip is then inserted into an analyzer and within a few minutes the saliva sample is checked and results delivered.
Nano-Bio-Chips deliver all the capabilities of a traditional laboratory but do not require expensive instrumentation to get results. Manufactured with techniques pioneered by the microelectronics industry, they have the potential to analyze large amounts of biomarker data at significantly lower cost than traditional tests, McDevitt said.
Chest pain brings about 5 million patients to U.S. emergency rooms each year, but 80 percent of those patients are not suffering heart attacks. Blood test results can take anywhere from 90 minutes to three hours, and in many cases it may be 12 to 24 hours before patients know whether or not they had a heart attack.
McDevitt said the new test could save lives, time and money by allowing doctors to identify those suffering from a heart attack before administering a battery of costly tests. "We hope to bend down U.S. health care costs through the marriage of electronics with diagnostic devices," he said.
"We believe that, in the future, we may be able to apply the same technology to improve screening for cardiovascular disease and diabetes, to identify problems before someone gets a heart attack," said Dr. Christie Ballantyne, chief of atherosclerosis and vascular medicine and professor of medicine at BCM and director of the Center for Cardiovascular Disease Prevention at the Methodist DeBakey Heart and Vascular Center.