Nanosystems Capture and Destroy Circulating Tumor Cells
(PhysOrg.com) -- Just as fly paper captures insects, a pair of nanotechnology-enabled devices are able to grab cancer cells in the blood that have broken off from a tumor. These cells, known as circulating tumor cells, or CTCs, can provide critical information for examining and diagnosing cancer metastasis, determining patient prognosis, and monitoring the effectiveness of therapies.
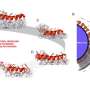
In a study published in the journal Angewandte Chemie International Edition, a team of investigators at the University of California, Los Angeles, developed a 1-by-2-centimeter silicon chip that is covered with densely packed nanopillars coated with an antibody that binds to a protein known as epithelial-cell adhesion molecule (EpCAM). EpCAM is expressed on the surface of a wide variety of solid-tumor cells but not by cells normally found circulating in the blood stream. The research team was led by Hsian-Rong Tseng, Ph.D., a member of the Nanosystems Biology Cancer Center, one of eight Centers of Cancer Nanotechnology Excellence established by the National Cancer Institute.
To test cell-capture performance, researchers incubated the nanopillar chip in a culture medium with breast cancer cells. As a control, they performed a parallel experiment with a cell-capture method that uses a chip with a flat surface. Both structures were coated with anti-EpCAM, an antibody protein that can help recognize and capture tumor cells. The researchers found that the cell-capture yields for the UCLA nanopillar chip were significantly higher; the device captured 45 to 65 percent of the cancer cells in the medium, compared with only 4 to 14 percent for the flat device.
The current gold standard for examining the disease status of tumors is an analysis of metastatic solid biopsy samples, but in the early stages of metastasis, it is often difficult to identify a biopsy site. By capturing CTCs, doctors may be able to perform a "liquid" biopsy, allowing for early detection and diagnosis, as well as improved treatment monitoring.
Meanwhile, a research team headed by Vladimir Zharov, Ph.D., of the University of Arkansas for Medical Sciences (UAMS), has developed a system that traps CTCs directly in the bloodstream, where they can then be removed by microsurgery or destroyed using a laser that does not harm the skin or other tissues. This work was published in two papers, one appearing the journal Biophotonics, the other in the journal Nature Nanotechnology. Dr. Lily Yang, Ph.D., of Emory University and a member of the Emory-Georgia Tech Center for Cancer Nanotechnology Excellence, also participated in this study.
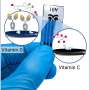
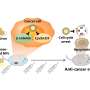
The UAMS system consists of two types of nanoparticles. The first is a magnetic nanoparticle designed to target a molecule known as urokinase plasminogen activator receptor. The second nanoparticle consists of gold-plated carbon nanotubes that target the folic acid receptor. Both receptors are found on many types of cancer cells but not on normal blood cells.
The investigators injected the two nanoparticle cocktail into mice bearing human breast tumors and then waited 20 minutes before using a combination of a magnet attached to skin above peripheral blood vessels to capture the labeled tumor cells and photoacoustic imaging to detect the gold-coated nanotubes that also label the captured tumor cells. "By magnetically collecting most of the tumor cells from blood circulating in vessels throughout the whole body, this new method can potentially increase specificity and sensitivity up to 1,000 times compared to existing technology," Dr. Zharov said.
The UCLA group's work, which is detailed in a paper titled, "Three-dimensional nanostructured substrates toward efficient capture of circulating tumor cells," was supported by the NCI Alliance for Nanotechnology in Cancer, a comprehensive initiative designed to accelerate the application of nanotechnology to the prevention, diagnosis, and treatment of cancer. An abstract of this paper is available at the journal's Web site.
The work from UAMS is detailed in two papers titled, "In vivo magnetic enrichment and multiplex photoacoustic detection of circulating tumour cells," and "Nanotechnology-based molecular photoacoustic and photothermal flow cytometry platform for in-vivo detection and killing of circulating cancer stem cells." This work was also supported in part by the National Cancer Institute's Alliance for Nanotechnology in Cancer. Abstracts of these papers are available at the respective journals' Web sites. [link 1, link 2]
Provided by National Cancer Institute