Combined dietary factors impact AMD risk; study finds glaucoma care cost-effective
Highlights of May’s Ophthalmology, the journal of the American Academy of Ophthalmology (Academy), include a new analysis of dietary factors and risks for age-related macular degeneration (AMD), and a landmark study on glaucoma treatment cost-effectiveness as linked to vision improvement and quality of life.
First Study of Combined Dietary Factors Finds Reduced AMD Risks
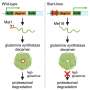
A diet that includes key nutrients and low-glycemic index foods is likely to reduce risks for age-related macular degeneration (AMD), according to the first study to analyze these factors in combination. Chung-Jung Chiu, PhD, of the Laboratory for Nutrition and Vision Research, Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University, led this new analysis of Age-Related Eye Disease Study (AREDS) data. The study team included AREDS researchers and was funded in part by the United States Department of Agriculture (USDA) and the National Institutes of Health (NIH). Earlier studies—including AREDS and the Nutrition and Vision Project of the Nurses’ Health Study—had revealed the AMD-protective effects of several nutrients and of a low-glycemic index (GI) diet, but Chiu’s study is the first to associate specific food intake patterns with substantial AMD risk reductions.
Study participants whose diets included higher levels of protective nutrients and of low-GI foods were at lowest risk for early and advanced AMD. This eye disease affects the retina, the sensitive tissue at the back of the eye that transmits images to the brain; advanced AMD can destroy the detailed, central vision people need to read, drive, and enjoy daily life. Data was analyzed for 4,003 AREDS participants, involving 7,934 eyes. Levels of AMD-protective nutrients, including vitamins C and E, zinc, lutein, zeaxanthin, omega-3 fatty acids (DHA and EPA), as well as low-GI foods, were assessed using participants’ food intake reports. (A food’s GI value is based on how fast its carbohydrates raise the body’s blood sugar levels; low GI foods have less impact on blood sugar fluctuations.) Each dietary factor was assigned a percentile score, and factor scores were added up to find each participant’s compound score. Compound scores were related to participants’ AMD risk, based on diagnostic eye photographs taken when they joined AREDS. Beta-carotene, assessed in this and earlier studies, did not affect risk levels in this analysis.
“Although the compound score may be a useful new tool for assessing nutrients in relation to AMD, specific dietary recommendations should be made only after our results are confirmed by clinical trials or prospective studies,” Dr. Chiu said.
AMD research is intensifying because the most susceptible population, people over age 60, is growing. A new report estimates 18 million will have AMD by 2050, 1.6 million of whom will be legally blind. Advanced AMD, especially the most prevalent “dry” form (geography atrophy), is a leading cause of severe vision impairment, and treatment options are limited. Preventing AMD and delaying disease progression would best preserve people’s quality of life while containing healthcare system cost and care challenges. Food sources of nutrients that support good general and eye health include: citrus fruits, vegetable oils, nuts, whole grains, dark green leafy vegetables, and cold water fish.
Glaucoma Treatment is Cost-Effective, US Study Finds
As the Obama administration pushes healthcare providers to compare treatments for value and efficacy, a study of glaucoma diagnosis and care in the United States reports for the first time that current practices are cost-effective in regard to both vision quality and quality of life. Primary-open angle glaucoma (POAG), the most common form of this potentially blinding eye disease, affects more than two million Americans annually. Many others—people with a family history of glaucoma or with elevated intraocular pressure (IOP), a known precursor—also receive screening and treatment services each year. Annual POAG-related health care costs now exceed $3 billion. David B. Rein, PhD, RTI International, collaborated on the study with researchers from the United States Centers for Disease Control and Prevention (CDC), Duke University and Harvard University. The study was funded by the CDC.
The researchers used a computer model to simulate assessment and treatment of POAG for 20 million people, tracked from age 50 to 100 (or death). Simulated participants were assigned ethnicities, gender, and life expectancy based on 2004 U.S. population data, and assigned active POAG, elevated IOP, and other relevant health conditions based on widely-accepted prevalence data. Patients diagnosed and treated for POAG were compared with people who were not assessed or treated. Care standards were drawn from the Academy’s Preferred Practice Pattern (PPP), used by U.S. and international ophthalmologists.
With no treatment a person with POAG would experience 5.2 years of visual impairment or blindness, on average, compared with 2.6 years for patients with treatment assumed to be conservatively effective. The peak age group for visual impairment and blindness was 75 to 79; with no treatment, 24.6 percent of people would have significant loss of vision, versus 12.1 percent (conservative efficacy) or 4.8 percent (optimistic efficacy) for treated patients.
Cost-effectiveness calculations included ophthalmic costs, nursing home costs attributable to vision problems, and total costs, as well as per-person Quality-Adjusted Life Years (QALY) and years of unimpaired vision. QALY is a multi-factor formula used by researchers to measure a person’s health improvement, general functionality and well-being following a medical intervention and is factored over the person’s estimated remaining years of life. The lower the dollar amount calculated for a QALY, the higher the value of the intervention. Compared with no treatment, routine POAG care cost $46,000 per QALY gained (conservative) or $28,000 per QALY gained (optimistic.) These results compared favorably with World Health Organization cost-effectiveness standards.
“Current glaucoma assessment and treatment patterns are cost-effective in reducing vision loss and associated health problems, even with routine eye exam costs included,” Dr. Rein said.
Source: American Academy of Ophthalmology