Epigenetic mark guides stem cells toward their destiny
(PhysOrg.com) -- Not all stem cells are completely blank slates. Some, known as adult stem cells, have already partially embraced their fates and are capable of becoming only cells of a particular type of tissue. So how do these tissue-specific stem cells restrict their fate? In research to appear in the March 20 issue of Cell, scientists at Rockefeller University have uncovered a gene-control mechanism that guides the development and differentiation of epidermal skin stem cells in mouse embryos and shown that this mechanism tempers the development of the skin barrier.
The work, led by Elaine Fuchs, head of the Laboratory of Mammalian Cell Biology and Development, and first author Elena Ezhkova, a postdoc in the lab, highlights the interactions between genetic and epigenetic regulators in embryonic skin stem cells and how these interactions change as stem cells begin the process of specialization. The findings also provide insights that could lead to therapeutic advance in treating prematurely born infants who have not yet fully formed the skin.
The skin is composed of two principle parts. The bottom 90 percent is known as the dermis; the outer 10 percent is the epidermis. The epidermis is composed of an inner layer (known as the basal layer) of dividing cells that gives rise to about 10 differentiated layers, the outermost of which is our body surface. “In contrast to embryonic stem cells, which can make all the cells of the body, epidermal stem cells restrict their options to making just these 10 differentiating layers,” explains Fuchs, who is also a Howard Hughes Medical Institute investigator and Rebecca C. Lancefield Professor at Rockefeller.
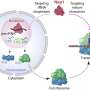
Clues as to how epidermal stem cells restrict their fate began to emerge when Ezhkova profiled the molecular makeup of the basal layer of the epidermis and compared it to the differentiating layers. As the skin stem cells began to differentiate, a complex of proteins (polycomb repressor complex) that restrict access to genes decreased their expression while a transcription factor (AP1), which activates genes, increased its expression.
Of the five major proteins that make up the polycomb repressor complex, Ezhkova focused on an enzyme called Ezh2. It has long been known that Ezh2 prevents cells from reading segments of chromosomes by adding a small modification that acts as a molecular clamp to the gene and physically blocks transcription factors from gaining access to them. Past research had shown that Ezh2 blocked access to skin differentiation genes in embryonic stem cells, but its role in skin stem cells had never been explored in a living animal.
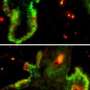
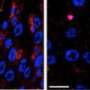
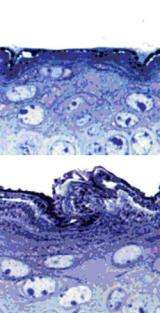
Working with Alexander Tarakhovsky, head of the Laboratory of Lymphocyte Signaling, Fuchs’s team bred mice with and without Ezh2 and found that mice without it were born with thicker skin than their normal counterparts. Without Ezh2 to block access to the skin differentiation genes, the skin stem cells began to differentiate much earlier. As a result, extra skin tissue builds up layer after layer.
Past research has shown that when embryonic stem cells lack Ezh2, genes for many cell differentiation pathways, not just the skin, lose their “molecular clamps” and become activated. In skin stem cells, however, these genes also lose these molecular clamps but only the skin differentiation genes become activated. To find out why only the skin pathway is switched on when the clamp is missing, the researchers found that AP1, the transcription factor that selectively activates skin differentiation genes, is present in both basal and differentiating skin cells. Without Ezh2, AP1 could bind and start to activate these genes in the basal layer, before the genes are normally expressed.
Another difference is that in embryonic stem cells, as soon as the molecular clamp is removed from muscle and neuronal genes, for example, an “activating mark” helps to switch on genes. In the skin stem cells this mark is not present on the non-skin genes, helping to keep them silent.
“Embryonic stem cells must be flexible — they produce all the cells of the animal,” explains Fuchs. “As development proceeds, the resident progenitors of developing tissues become increasingly more restricted in their repertoire of differentiation programs. As the embryo develops, tissue-specific stem cells seem to remove the activating mark on those programs that will never be used, thereby switching off the wrong programs permanently.” Then, to activate the right programs, the genes become dependent upon tissue-specific transcription factors.”
The system is clearly more complicated than this,” Fuchs adds, “but the result is a series of intrinsic and extrinsic factors that control gene expression.”
More information: Cell 136(6): 1122—1135 (March 20, 2009) Ezh2 Orchestrates Gene Expression for the Stepwise Differentiation of Tissue-Specific Stem Cells; Elena Ezhkova, H. Amalia Pasolli, Joel S. Parker, Nicole Stokes, I-hsin Su, Gregory Hannon, Alexander Tarakhovsky and Elaine Fuchs
Provided by Rockefeller University (news : web)